Journal Information
Vol. 60. Issue 7.
Pages 448-450 (July 2024)
Vol. 60. Issue 7.
Pages 448-450 (July 2024)
Scientific Letter
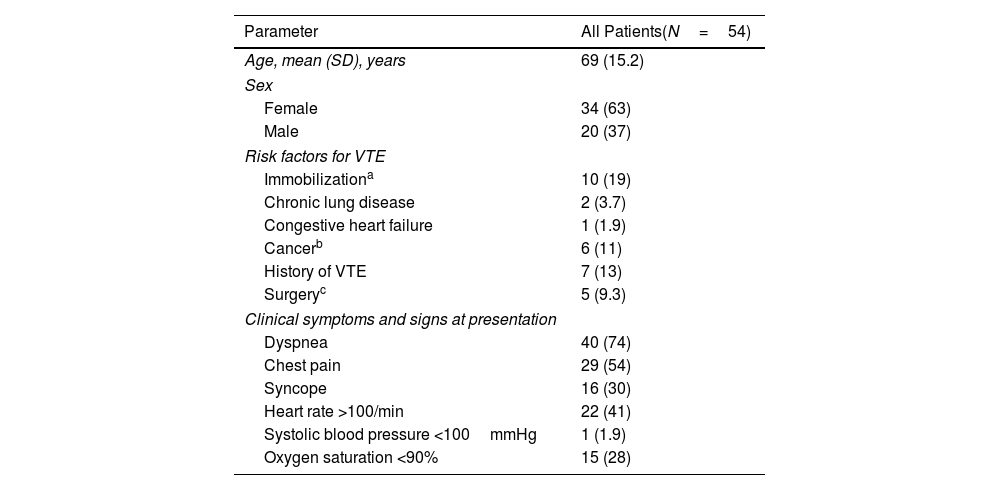
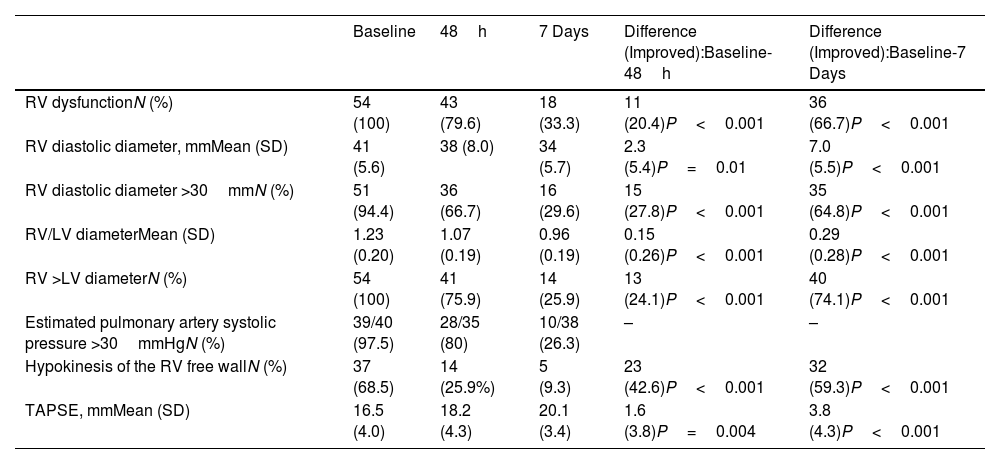
Time to Resolution of Right Ventricle Dysfunction in Patients With Acute Pulmonary Embolism
Visits
740
Winnifer Briceñoa, Gema Díazb, Ana Castilloa, Ignacio Jaraa, Edwin Yonga, Laura Lagoa, Mads Dam Lyhnec,d, Manuel Monreale,f, Behnood Bikdelig,h,i, David Jimeneza,f,j,
Corresponding author
a Respiratory Department, Hospital Ramón y Cajal and Instituto Ramón y Cajal de Investigación Sanitaria IRYCIS, Madrid, Spain
b Respiratory Department, Hospital Puerta de Hierro, Madrid, Spain
c Department of Anesthesiology and Intensive Care, Aarhus University Hospital, Denmark
d Department of Clinical Medicine, Aarhus University, Denmark
e Chair for the Study of Thromboembolic Disease, Faculty of Health Sciences, UCAM – Universidad Católica San Antonio de Murcia, Spain
f CIBER Enfermedades Respiratorias (CIBERES), Madrid, Spain
g Cardiovascular Medicine Division, Brigham and Women's Hospital, Harvard Medical School, Boston, MA, USA
h Center for Outcomes Research and Evaluation (CORE), Yale University School of Medicine, New Haven, CT, USA
i Cardiovascular Research Foundation, New York, USA
j Medicine Department, Universidad de Alcalá, Madrid, Spain
Ver másThis item has received
Article information
These are the options to access the full texts of the publication Archivos de Bronconeumología