Sarcoidosis is a chronic multi-systemic granulomatous disease of unknown origin, characterized by the appearance of multiple epithelioid granulomas in different organs. It has typically been described in cancer patients, before, during or after their diagnosis of malignant disease.1 In contrast, a sarcoid-like reaction (SR) is considered a specific entity, consisting of a sarcoid-like syndrome caused by a crossover reaction to circulating tumor antigens in some cancer patients.2 We report a case of SR in a cancer patient detected during the differential diagnostic process of suspected metastatic dissemination of the primary tumor.
This was a 32-year-old man with a history of testicular germ cell tumor (embryonal carcinoma) detected in 2009, treated with surgery and chemotherapy, with no evidence of local or distant tumor relapse. In follow-up, a whole-body computed tomography (CT) performed 6 years after diagnosis revealed a symmetric radiological pattern of bilateral mediastinal and hilar lymphadenopathies (Fig. 1A) and bilateral pulmonary nodules (Fig. 1B). In view of these radiological findings, a differential diagnosis of either metastatic tumor dissemination or SR was proposed. The latter seemed more likely, given the radiological pattern and the long period (6 years) without evidence of malignant disease. To reach a definitive diagnosis, we first performed a biopsy of one hilar lymphadenopathy by endobronchial ultrasound, which was found on histology to be consistent with SR. Secondly, we decided to perform a surgical biopsy of several pulmonary nodules using video-assisted thoracoscopy, which were also confirmed on histology to be SR (Fig. 1C).
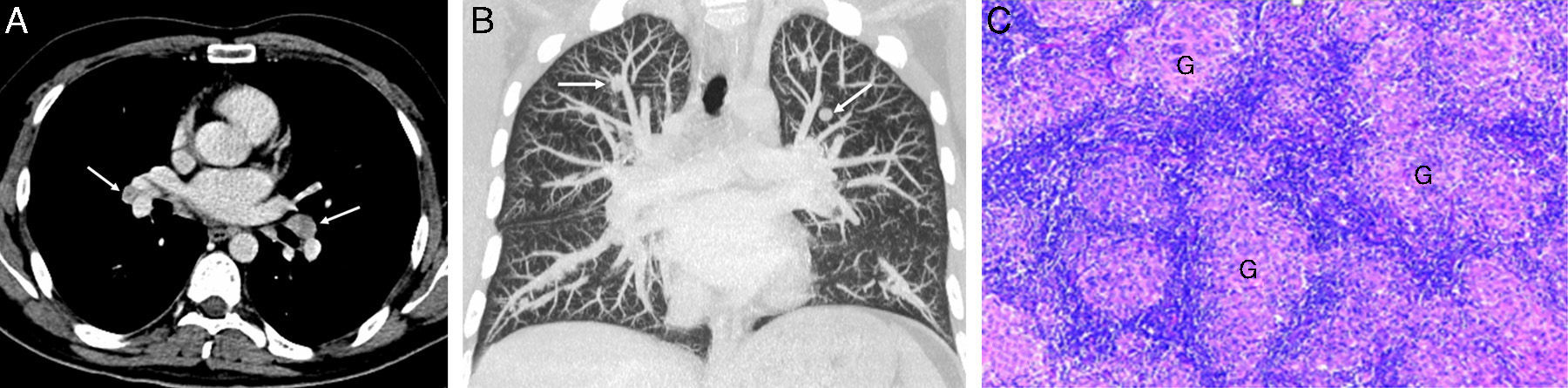
(A) Axial chest CT (mediastinal window) showing symmetrical bilateral hilar lymphadenopathies (arrows). (B) Coronal maximum intensity projection of chest CT (pulmonary parenchymal window) revealing bilateral pulmonary nodule, predominantly in the upper lobes (arrows). (C) Histological image of a pulmonary nodule resected by video-assisted thoracoscopy showing non-necrotizing granulomas (G) formed by epithelioid histiocytes with no neoplastic cellularity.
Cases have been described in the literature of patients with testicular cancer who have developed SR during their oncological follow-up, in the absence of local tumor recurrence or distant metastasis. The relationship between SR and testicular cancer is controversial, partly because both diseases occur in young men, so the association may, to a certain extent, be coincidental.3,4 Patients with SR generally have a symmetrical radiological pattern of bilateral hilar and mediastinal lymphadenopathies, while concomitant bilateral pulmonary nodules are less common. In a recent review of SR in patients with testicular cancer, it was observed that: (1) involvement is mild and basically limited to the mediastinum and the lung; (2) it can resolve spontaneously without specific treatment (indeed, most patients did not receive corticosteroids), and (3) chemotherapy is not a criterion for appearance.5
The appearance of intrathoracic lymphadenopathies and pulmonary nodules in patients with testicular cancer is a diagnostic challenge with significant therapeutic repercussions. SR should be suspected if metastatic disease is not detected in other sites, and it is essential that a definitive histological diagnosis is reached using fiberoptic bronchoscopy/endobronchial ultrasound and/or video-assisted thoracoscopy. To assume the presence of metastatic disease without histological confirmation would involve exposing the patient to unnecessary chemotherapy, and even worse, the failure of the granulomatous disease to respond to chemotherapy would lead to the use of more aggressive second-line therapies with greater side effects.
We believe that awareness of SR as a syndrome that can simulate metastatic disease in some patients with testicular cancer is essential for optimal management, and for avoiding unnecessary chemotherapy. Cases in which SR is suspected on radiology must always be confirmed by histology.
Please cite this article as: Ureña-Vacas A, Pinilla-Pagnon I, Gorospe Sarasúa L. Reacción sarcoidea con afectación mediastínica y pulmonar en paciente con antecedente de cáncer testicular. Arch Bronconeumol. 2017;53:77–78.