Intravesical instillation of bacillus Calmette-Guerin (BCG), a live attenuated strain of Mycobacterium bovis, has been shown in numerous studies to be an effective treatment for superficial in situ bladder cancer. However, this procedure is not free of complications.1–3
We report the case of a patient diagnosed with pleural effusion due to M. bovis after treatment with intravesical BCG instillation.
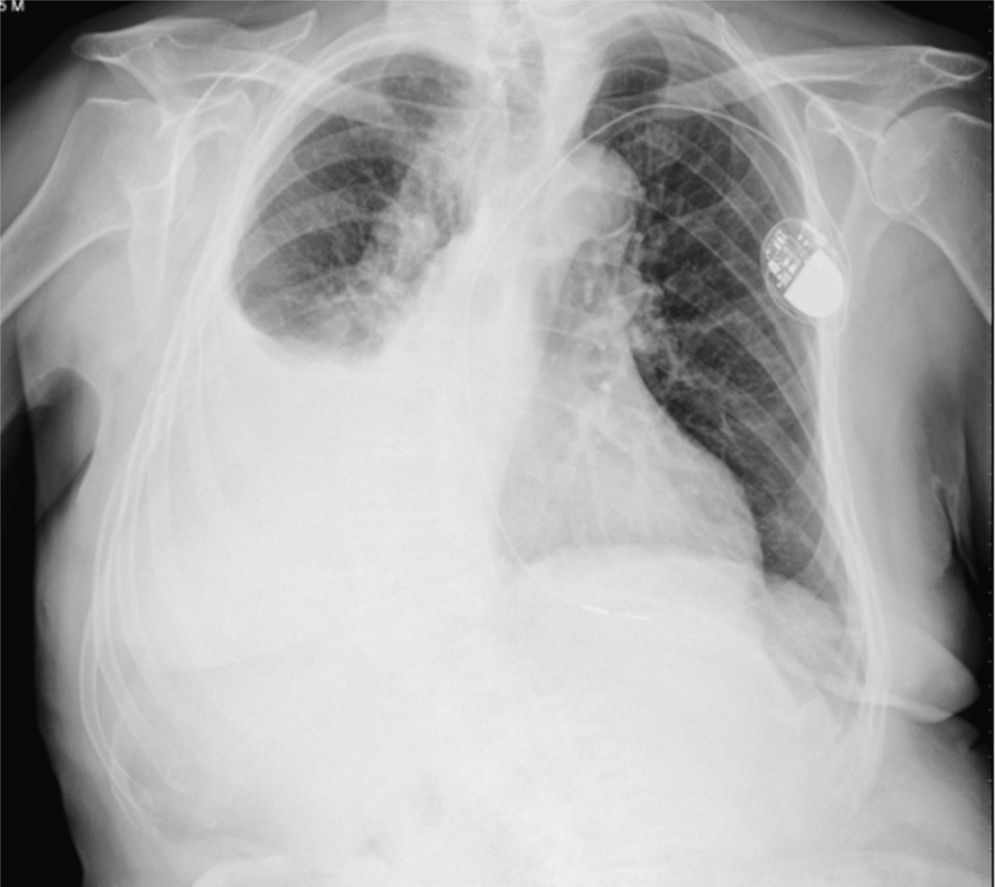
This was an 85-year-old man, former smoker, with mild chronic obstructive pulmonary disease, atrial fibrillation, and pacemaker implantation due to sick sinus syndrome, diagnosed with multifocal transitional cell carcinoma of the bladder treated by transurethral resection and 6 BCG instillations. One year later, he presented in the emergency department with pleuritic chest pain and increased dyspnea. Chest radiograph (Fig. 1) revealed right pleural effusion. Empirical antibiotic therapy began with amoxicillin/clavulanic acid and the patient was admitted to the respiratory medicine department for further examination with chest computed tomography (CT) and diagnostic thoracentesis. The CT revealed extensive right pleural effusion with passive atelectasis of the ipsilateral lower lobe, subpleural calcified granuloma in the left lower lobe, and prevascular and hilar lymphadenopathies, suggestive of a previous granulomatous process. Thoracentesis was performed, yielding cloudy pleural exudate with elevated adenosine deaminase (ADA) (63.9U/l), and a predominance of mononuclear cells (85%). We did not perform a pleural biopsy due to the high probability that this was a Mycobacterium infection, given the characteristics of the pleural fluid. Culture of the fluid was positive for M. bovis, leading to a diagnosis of pleural effusion due to M. bovis caused by intravesical instillation of BCG. The patient was treated for 6 months with isoniazid, rifampicin, and ethambutol with good clinical response and resolution of the pleural effusion, with no adverse drug effects.
Although intravesical instillation of BCG is usually well tolerated, local (1%) and systemic (4.8%) complications have been described. Among the systemic events, pulmonary complications account for 1%–3% and 5 forms of presentation have been described: interstitial pneumonitis, empyema, diffuse alveolar damage, pneumonia with or without cavitation, and miliary tuberculosis (TB). The latter is the most common form of infection due to BCG in the literature and accounts for one third of cases.1,2 Some authors argue that the underlying cause of systemic involvement is hypersensitivity to the BCG, while others believe that it is due to systemic dissemination after hematogenous seeding from the bladder.3,4
No evidence is available to show that prophylaxis with isoniazid protects against systemic dissemination after intravesical BCG administration.5 Complications may take months or even years to appear after the first instillation.2
In our patient, culture was positive for M. bovis. The chest CT showed residual lesions suggestive of an old untreated TBC. Complications occur more often in patients with a history of TBC than in patients without previous tuberculous disease.6
Our case was an unusual presentation of bacilli in the pleural fluid, prompting a diagnosis of pleural effusion due to BCG dissemination after intravesical instillation, 1 year after receiving this treatment. It is also uncommon for this complication to present as pleural effusion. We could only find 1 similar case of pleural effusion 6 years after administration of BCG treatment, although in that patient, no mycobacteria could be isolated from pleural fluid.7
Please cite this article as: Roca Noval A. Derrame pleural tras tratamiento intravesical con bacilo de Calmette-Guérin. Arch Bronconeumol. 2017;53:694–695.