Although muscle tissue makes up more than 50% of the total body mass, metastatic extension to the skeletal muscle is an exceptional event in solid organ neoplasms, with an accumulated incidence of less than 1.5% in recent series, and it is usually limited to advanced phases of the disease.1–3 Due to their clinical and radiological appearance, skeletal muscle metastases (SMM) are similar to soft tissue sarcomas, entities with greater prevalence in which case surgical resection offers potentially curative results.2 This differential diagnosis takes on special relevance if the SMM is the initial manifestation of a primary tumor that had been clinically silent up until that moment, a situation that has been infrequently reported in the literature.4–6
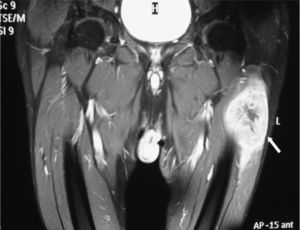
Our patient is a 69-year-old male ex-smoker, whose medical history included the presence of arterial hypertension, dislipidemia and polymyalgia rheumatica. The patient reported the appearance of a tumor on the left thigh, with slow progressive growth and accompanied by continuous dull pain. With the exception of an unquantified weight loss, the patient denied any other systemic symptoms. After several weeks, he also reported the appearance of a second smaller lesion on his right calf. The physical examination showed that the patient was in a state of good general health, with no findings on the cardiopulmonary auscultation or palpable lymphadenopathies. On the outer side of the left thigh, there was a stone-like mass that was not painful to touch (10cm×5cm), with scarce mobility on deeper planes and no signs of local inflammation, which was covered with skin that was intact. A second lesion (2cm×1cm) with similar characteristics was on the right gastrocnemius. Magnetic resonance imaging (MRI) with a contrast revealed a large, very heterogeneous mass that was sarcomatous in appearance on the vastus externus muscle of the left thigh (Fig. 1), and a smaller-sized mass in the lateral gastrocnemius of the right leg. A cytology obtained from this latter lesion, using fine-needle aspiration (FNA), was consistent with a poorly differentiated carcinoma. Later, an incisional biopsy of the thigh mass confirmed infiltration by an epidermoid carcinoma with complex epithelial phenotype in the immunohistochemistry study (positivity for high molecular weight keratins, pankeratins AE1–AE3, thrombomodulin, carcinoembryonic antigen and p63). The study was completed with a thoracoabdominal computed tomography study that revealed multiple bilateral pulmonary nodules indicative of metastasis, among which there was a larger lesion in the right upper vertex (3cm×3.2cm) with spiculated contours that was identified as a probable primary tumor. By means of transthoracic FNA, a sample was obtained, whose cytological study was compatible with a scarcely differentiated carcinoma. With the determination of the lesion as a stage IV non-small-cell lung cancer (NSLC), the patient underwent palliative chemotherapy (cisplatin and docetaxel). Despite the initial decrease in size of the SMM after 6 cycles of treatment, the tumor progression was confirmed 10 months later in the lungs, brain and liver. At that moment, we opted for symptom management.
Various mechanisms have been invoked to justify the apparent resistance of the muscles to the metastatic infiltration, among which there are mechanical factors (tissue pressure), metabolic factors (production of lactic acid and oxygen free radicals, local pH) and immunological factors.2 The primary tumor that is most frequently involved in the majority of series is bronchogenic carcinoma, followed by gastrointestinal and urothelial neoplasms.1,3 From a clinical standpoint, SMMs usually present as nodules or painful masses with signs of local inflammation, and among their most frequent locations are the lower extremities, the chest wall and the paravertebral musculature.1–3 MRI is the radiological technique of choice, even though its typical findings (tissue hyperintensity in the T2 sequences, signal reduction in T1 sequences and irregular captation of gadolinium) are relatively unspecific.1,2 Therefore, when using this diagnostic approach, it is crucial to also have a histological exam, which, on occasions, should be completed with immunohistochemistry techniques given the limited differentiation that the SMM can exhibit. An exhaustive review of the literature identified 114 cases of NSLC associated with SMM, with a mean survival of 6 months; the existence of a single metastasis and its metachronic presentation with the primary tumor defined a subgroup of patients with better prognoses.2 In this as well as in other series, the initial presentation of NSLC in the form of SMM in the lower extremities, with no evidence of previous dissemination to other anatomically more predictable locations, is very infrequent.1,4–6 This present case illustrates the need, in cases with similar scenarios, to carry out a complete extension study with histological determination which can exclude other more prevalent situations, particularly the possibility of a soft tissue sarcoma with lung metastasis, given the therapeutic implications of this differential diagnosis.
The authors would like to thank Dr. Ana Belén Enguita-Valls, from the Pathological Anatomy Department of the Hospital Universitario 12 de Octubre, for her collaboration in the development of this manuscript.
Please cite this article as: Fernández-Ruiz M, et al. Metástasis en músculo esquelético como presentación inicial de un carcinoma no microcítico de pulmón. Arch Bronconeumol. 2011;47:422–3.