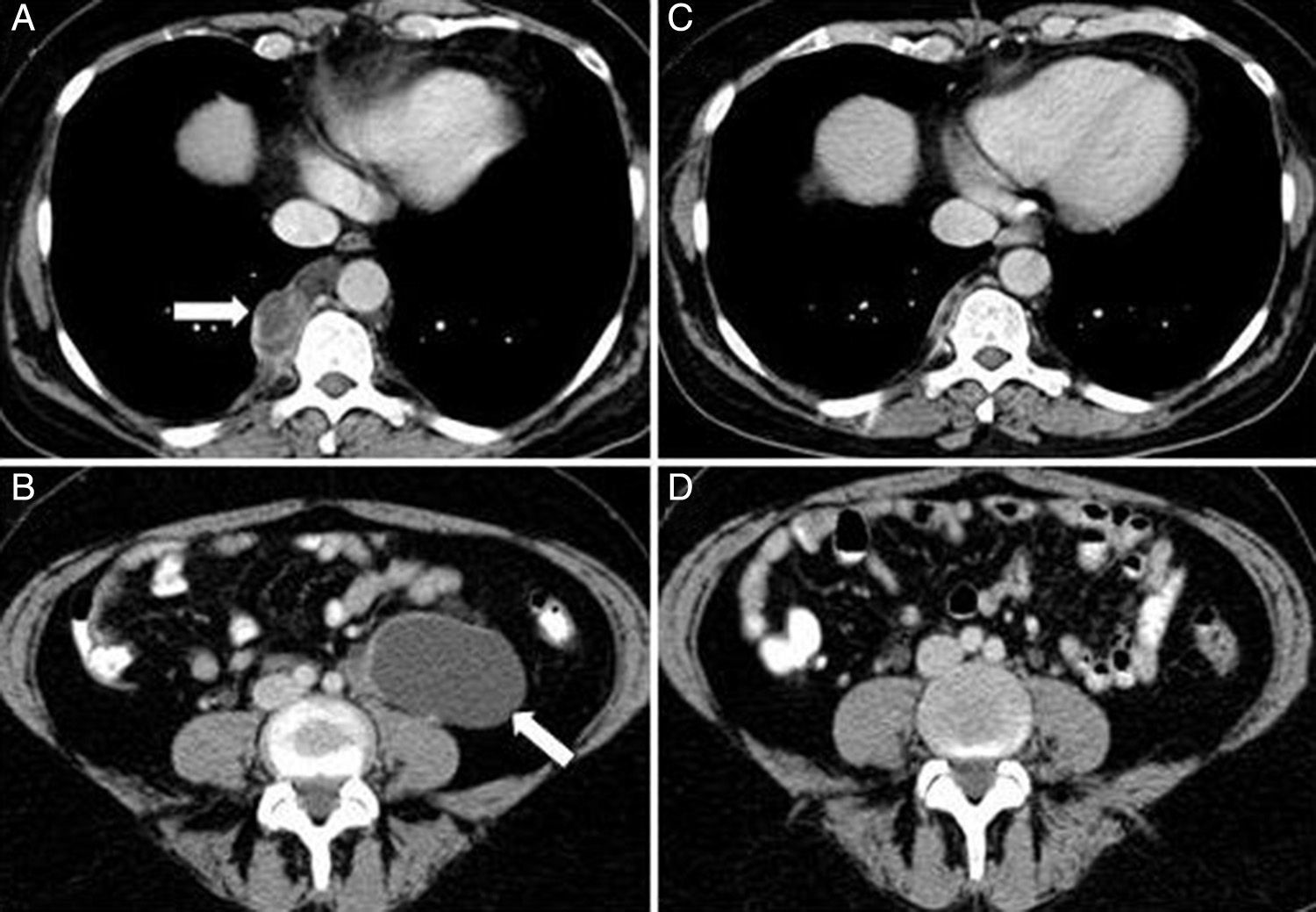
A 53-year-old woman was diagnosed with lymphangioleiomyomatosis (LAM) in 2010, presenting diffuse pulmonary involvement with multiple fine walled cysts, right retrocrural cystic lymphangioleiomyomas, and multiple retroperitoneal tumors of cystic appearance, consistent with abdominal lymphangioleiomyomas, the largest being 6.8×3.9×5.1 in diameter (Fig. 1 A and B). Lung function on diagnosis showed forced vital capacity (FVC) 3300ml (98%), forced expiratory volume in 1 second (FEV1) 2370ml (82%) and an FEV1/FVC ratio 69%. Carbon monoxide diffusing capacity (DLCO) was 89%. She reported symptoms of dyspnea on heavy exertion and intermittent episodes of predominantly catamenial chest and abdominal pain. After 2 years of follow-up, lung function had significantly worsened, with FEV1 2040ml (71%) and DLCO 72%, increased basal dyspnea, and catamenial symptoms persisted. In view of her clinical and functional progression, treatment was started with the mammalian target of rapamycin (m-TOR) inhibitor sirolimus at a dose of 2mg/day.1 One year after beginning treatment, a follow-up radiological examination showed practically complete resolution of the thoracic and abdominal lymphangioleiomyomas2 (Fig. 1C and D). Clinical improvement and stabilized lung function were observed, with FEV1 1980ml (70%) and DLCO 82%. This image shows the beneficial effect of sirolimus in reducing the size of the thoracic and abdominal lymphangioleiomyomas, and in stabilizing lung function in patients with LAM.
Chest computed axial tomography (CAT) (A) showing a right paravertebral cystic lesion 3.2×1.9cm, consistent with retrocrural lymphangioleiomyoma. Abdominal CAT (B) showing tumor 6.8×3.9×5.1cm of retroperitoneal cystic appearance, located in the left para-aortic region, extending to the pelvis, consistent with abdominal lymphangioleiomyoma. Chest-abdominal CAT one year later (C and D) showing practically complete resolution of lesions.
Please cite this article as: Cabeza Osorio L, Ruiz Cobos MÁ, Casanova Espinosa Á. Resolución de los linfangioleiomiomas torácicos y abdominales en una paciente con linfangioleiomiomatosis tratada con sirolimus. Arch Bronconeumol. 2016;52:329–330.