Respiratory day hospitals (RDH) are a useful alternative form of hospitalization.1 However, no studies are available that demonstrate their suitability for managing exacerbations in patients with severe respiratory disease. In this communication, we report our experience in this area.
Between December 2013 and November 2014, we performed an observational, longitudinal, quasi-experimental study (patients were their own controls) of all patients who attended the RDH (2 or more admissions/emergency visits due to decompensation of an underlying respiratory disease in the previous year). All patients were followed for 1 year, and data from the previous year were obtained from their clinical records. The study was approved by the Ethics Committee (no. 2016/424). Widely accepted criteria were used to establish the diagnosis of COPD, asthma, and bronchiectasis, and to determine levels of physical activity, dyspnea grade, deterioration of state of health, BODE index, 6-minute walk test, classification of COPD patients, and definition of sepsis.2–12
A descriptive analysis was conducted of patient characteristics, and visits to the emergency department/hospitalizations between the year prior to and the year after the patient's first visit to the RDH were compared using the Wilcoxon non-parametric test for paired data, and variables associated with hospitalization were studied. It was estimated that the mean annual number of events (emergency visits and admissions) in these patients would be 9–10, and that after implementation of the RDH this rate could be reduced by 25%. To achieve a power of 85%, 125 patients would be needed to detect significant differences (p<0.05) between the number of events before and after RDH.
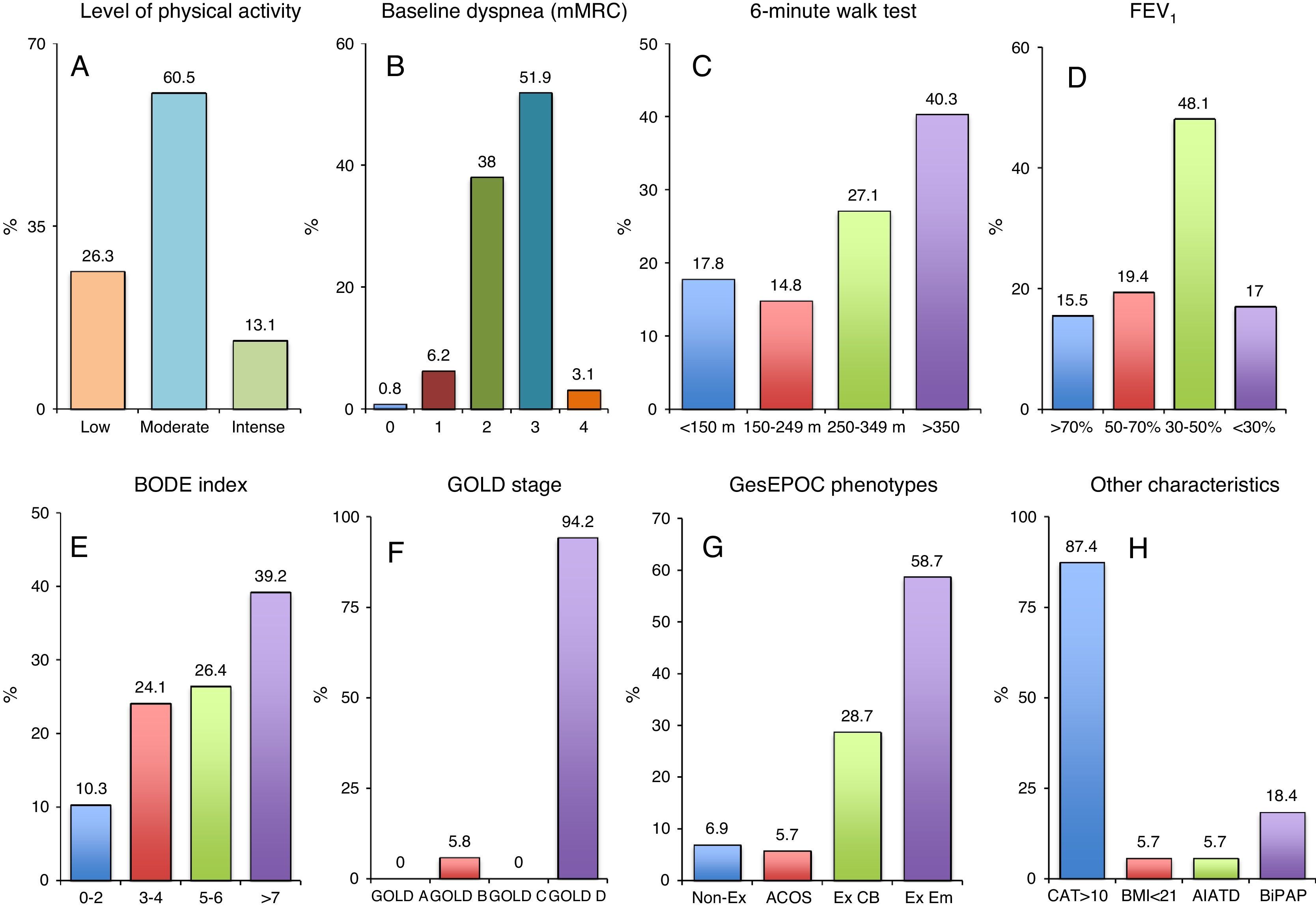
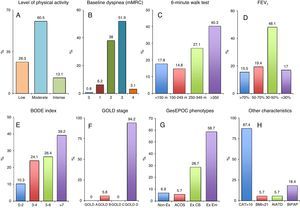
During the study period, 1053 visits to the RDH for exacerbations were recorded in 129 patients (COPD [87], bronchiectasis [12], asthma [7], and others [23]). Fig. 1 shows the level of physical activity (low/moderate in 112/129) (Fig. 1A), dyspnea grade (mMRC 34 in 71/129) (Fig. 1B), 6-minute walk test (42/129 walked<250m) (Fig. 1C), and FEV1 (84/129<50%) of the overall study population (Fig. 1D). Among COPD patients, 57/87 had a BODE index>4 (Fig. 1E), 82/87 were GOLD stage D (Fig. 1F), 76/87 had a GesEPOC exacerbator phenotype (Fig. 1G), 76/87 had CAT≥10, 5/87 had a body mass index<21, 5/87 had alpha-1 antitrypsin deficiency, and 16/87 were receiving BiPAP home oxygen therapy (Fig. 1H). In total, 8.6% of visits (91/1053) required hospital admission, mainly due to the need for intravenous antibiotics (25; 27.5%), acute respiratory failure (21; 23.1%), and failure of previous outpatient therapy (12; 13.2%). When the year prior to and the year after the first visit to the RDH were compared, a reduction in both the number of visits to the emergency room (110 vs 57; P=.001), and in the number of hospital admissions (236 vs 183; P=.006) was observed. Results were similar when data from patients who died during the follow-up year (19; 14.7%) were excluded: 90 vs 43 visits to the emergency room (P=.002); and 190 vs 141 hospital admissions (P=.003). Moreover, 81.8% (45/55) of patients receiving continuous home oxygen therapy had COPD.
(A) Level of physical activity, (B) dyspnea grade, (C) 6-minute walk test, and (D) FEV1 in the overall study population. (E) BODE index, (F) GOLD stage, (G) GesEPOC phenotype, (H) CTA, body mass index, alpha-1 antitrypsin deficiency, and BiPAP home therapy in COPD patients. A1ATD: alpha-1 antitrypsin deficiency; BiPAP: bilevel positive airway pressure; BMI: body mass index; CAT: chronic obstructive pulmonary disease assessment test; CB: chronic bronchitis; Em: emphysema; Ex: exacerbator; mMRC: modified Medical Research Council.
A multivariate analysis of COPD patients found that factors associated with a greater risk of admission were respiratory acidosis (OR 9.67, 95% CI: 1.48–62.9), diabetes mellitus (OR 2.01; 95% CI: 1.08–3.77), low blood pressure (OR 0.99; 95% CI: 0.97–1.00), tachycardia (OR 1.02; 95% CI: 1.00–1.04), diuretic failure (OR 19.7; 95% CI: 4.32–89.8), isolation of a multiresistant microorganism in sputum (OR 4.41; 95% CI: 2.06–9.42), sepsis (OR 4.01; 95% CI: 1.16–13.8), and use of accessory muscles (OR 4.94; 95% CI: 2.60–9.40).
This study confirms that even in the first year of functioning, the RDH can reduce pressure on the emergency department and the number of admissions, despite the advanced respiratory disease status and high comorbidity burden of the patients seen. Moreover, it shows that certain factors are associated with a higher risk of admission among COPD patients. Our results coincide with those of other studies,1,13,14 although our series differs in that that most of our patients had very severe disease and presented higher exacerbation rates.
The significant reduction, in both the number of visits to the emergency room (110 vs 57; P=.001), and the number of hospital admissions (236 vs 183; P=.006) compared to the previous year appears to confirm the efficacy of the RDH. These results may be directly associated with the more specialized care provided the RDH doctors and nurses in the management of the respiratory patient.
The opening hours of the RDH are limited and a patient's destination must be decided within a few hours, so we examined which factors in COPD patients might predict hospitalization, to be able to anticipate their final destination. Some of the factors we identified are indicative of very severe COPD exacerbations11: patients who may need ventilation (acidosis) or who have hemodynamic instability (tachycardia and hypotension).
The limitations of this study are: (1) no strict protocol for reevaluation of each exacerbation (all patients were seen 72 hours after an exacerbation,11 but some had to be seen several times); (2) use of an mMRC scale for evaluating dyspnea in all patients although it is only validated for COPD. We decided to use this tool because it is easy to apply and because it is usually collected in the emergency department; and (3) lack of a cost-effectiveness study.
In short, a RDH can constitute an alternative to conventional hospitalization, and is suitable for the outpatient management of a large number of respiratory exacerbations, even in severe patients. COPD patients present a series of factors that predict a greater risk of hospital admission.
Please cite this article as: Lourido-Cebreiro T, Rodríguez-García C, Gude F, Valdés L. ¿Es útil un hospital de día de enfermedades respiratorias en pacientes graves? Arch Bronconeumol. 2017;53:400–402.