Hydatid cyst disease (hydatidosis or echhinococcosis) is a parasitic disease found in farming communities, notably in South America, North Africa, the Middle East, the Mediterranean and Eastern and Central Anatolia.1 It is most frequently seen in the liver (60%–70%) and lungs (20%–30%). Intrathoracic extrapulmonary involvement is rare.2 The rate of recurrence following surgical removal of lung or liver hydatid cystis has been to be between 1.4% and 11%.3 This report describes a case of a hydatid cyst imitating thoracic wall malignancy.
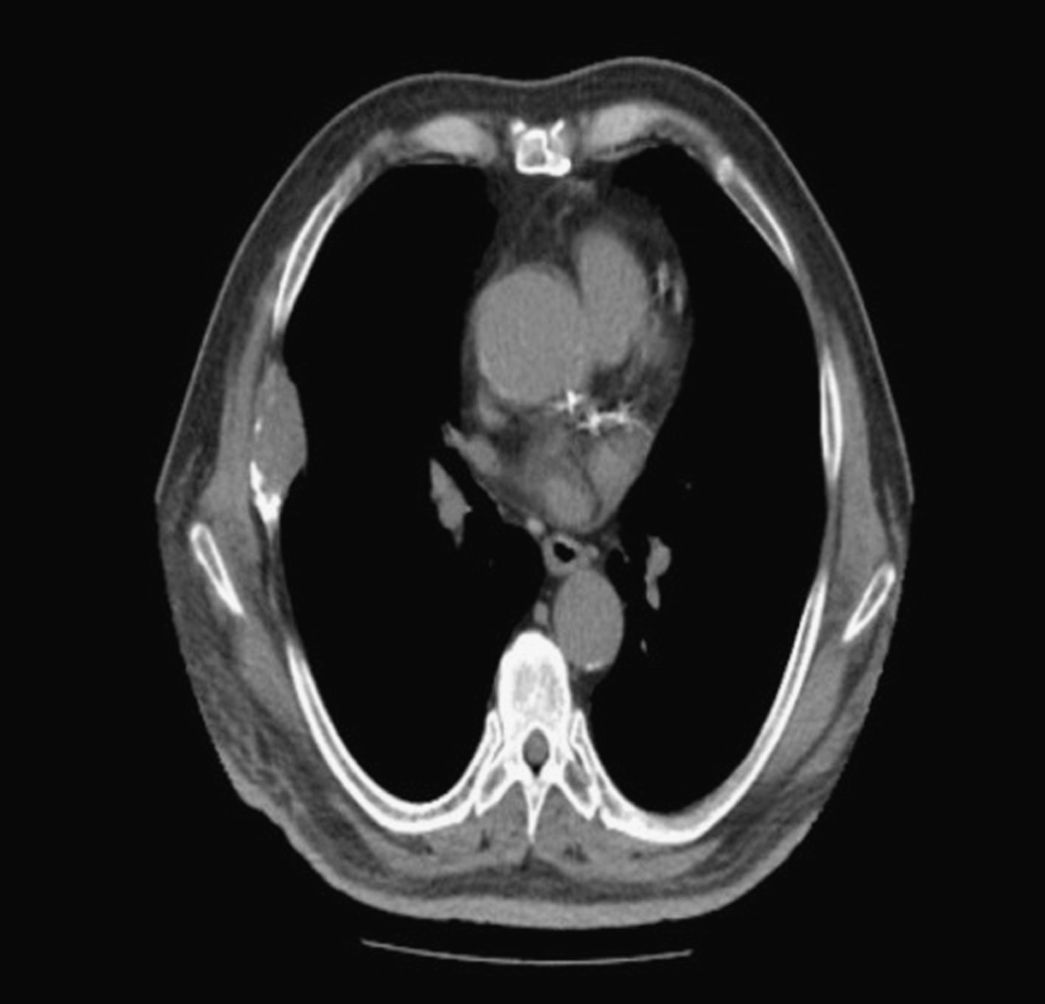
A 67-year-old male, non-smoker, a native of Ağrı (Eastern Anatolia), was admitted to our clinic with a 3-month history of cough and loss of appetite. Physical examination showed diminished breath sounds. Laboratory findings were within normal limits. Chest X-ray revealed a homogenous density adjacent to the right chest wall. Chest computed tomography (CT) showed a 52×28mm extrapleural mass in the thoracic wall destroying the anterior right sixth rib (Fig. 1). Suspecting thoracic wall malignancy, transthoracic fine needle aspiration biopsy (TTFNAB) was performed. The cytology report indicated “homogenous eosinophyllic lamellar material of a hydatid cyst closely surrounded by scolices”. The patient underwent surgery to remove the cyst. Postoperative 15–20mg/kg/day albendazol treatment was initiated and finalized at 12 weeks. After 2 years of follow-up, the patient has not shown any sign of recurrence.
Hydatid cyst disease is usually asymptomatic, and is diagnosed after combined clinical, radiological, and specific laboratory tests.4 The metastasis of hydatid cyst in costa is generally slow, and laboratory tests are usually negative. In our case, specific laboratory studies for hydatid cyst were not performed, since thoracic wall tumor (osteosarcoma) was strongly suspected on the CT image of rib destruction, and TTFNAB was used to establish definitive diagnosis, even though guidelines recommend avoiding this technique in order to prevent tumor spread and minor or major allergic reactions.
In cases of recurrence of chest wall hydatid cyst, the fundamental principle in surgical therapy is the removal of the affected ribs or the chest wall.5 In our case the affected sixth rib was partially removed.
Treatment with mebendazole or albendazole is effective for pulmonary hydatid cysts in up to 70% of cases. Antihelmintics are known to cause degenerative changes in the cyst membrane and cyst rupture. Unlike the liver, the lung environment is not aseptic, so even if the parasite perishes, cyst membrane persisting in lung cavities can lead to secondary bacterial infection and other complications, including anaphylactic reaction, asphyxia, tension pneumothorax and massive hemoptysis. Preoperative albendazole may increase the risk of perforation in cases of pulmonary hydatid cysts, and we do not recommend this therapy. Medical treatment is recommended for patients who can not tolerate or who do not accept surgery.5 In our case, the treatment was finalized with postoperative oral albendazol.
Thoracic wall involvement in hydatid cyst disease is rare. For this reason, we believe this description of a definitive diagnosis of this phenomenon to be of interest, particularly in areas where hydatid disease is more frequently encountered.