A 20-year-old man presented in the emergency room with a severe asthma exacerbation. His history was significant for extrinsic asthma with sensitization to pollens and dust mites, poorly controlled since childhood, smoker from the age of 14 years, with no consumption of other toxic substances, and no history of surgical interventions.
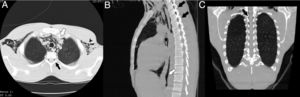
Given his clinical symptoms and radiological images suggestive of pneumomediastinum, computed tomography was performed, confirming pneumomediastinum dissecting the trachea, bronchi, esophagus, vena cava, and prevascular space to the diaphragm, with no evidence of pneumothorax or other lesion. Air was incidentally observed in the spinal canal between the cervical vertebrae and the last thoracic vertebrae (Fig. 1).
Pneumorrhachis or presence of air in the spinal canal is detected in 1/30000 patients in hospital emergency departments.1 It can be iatrogenic, traumatic, or non-traumatic. It is often described as an incidental finding in images obtained in association with traumatic pneumothorax and subcutaneous emphysema, and less frequently with non-traumatic or spontaneous pneumopericardium or pneumomediastinum.
Standard X-ray is the imaging technique of choice when pneumomediastinum is suspected, but tomographic techniques may be useful for observing associated changes, such as pneumorrhachis.
Both findings are benign processes2 that resolve spontaneously within 2–3 weeks.
Please cite this article as: Gutiérrez-Morales I, Gallego-Borrego J, Gutiérrez-Tello M, Fernández-Recio M, Romero-Ruiz F. Neumorraquis cervicotorácico y neumomediastino espontáneo en adulto con agudización asmática. Arch Bronconeumol. 2019;55:588.