A 71-year-old man presenting at our emergency department due to a 6-day clinic of fever of up to 38.9°C, oropharyngeal dryness secondary to COVID-19 pneumonia.
In the preliminary evaluation it was observed an increase in the D-Dimer values (4670μg/L). Computed Tomography Pulmonary Angiography (CTPA) showed a segmental pulmonary thromboembolism (PTE) in LSD and multiple peripheral bilateral ground glass opacities compatible with viral pneumonia. CTPA also showed bilateral varicose bronchiectasis (Fig. 1A and B).
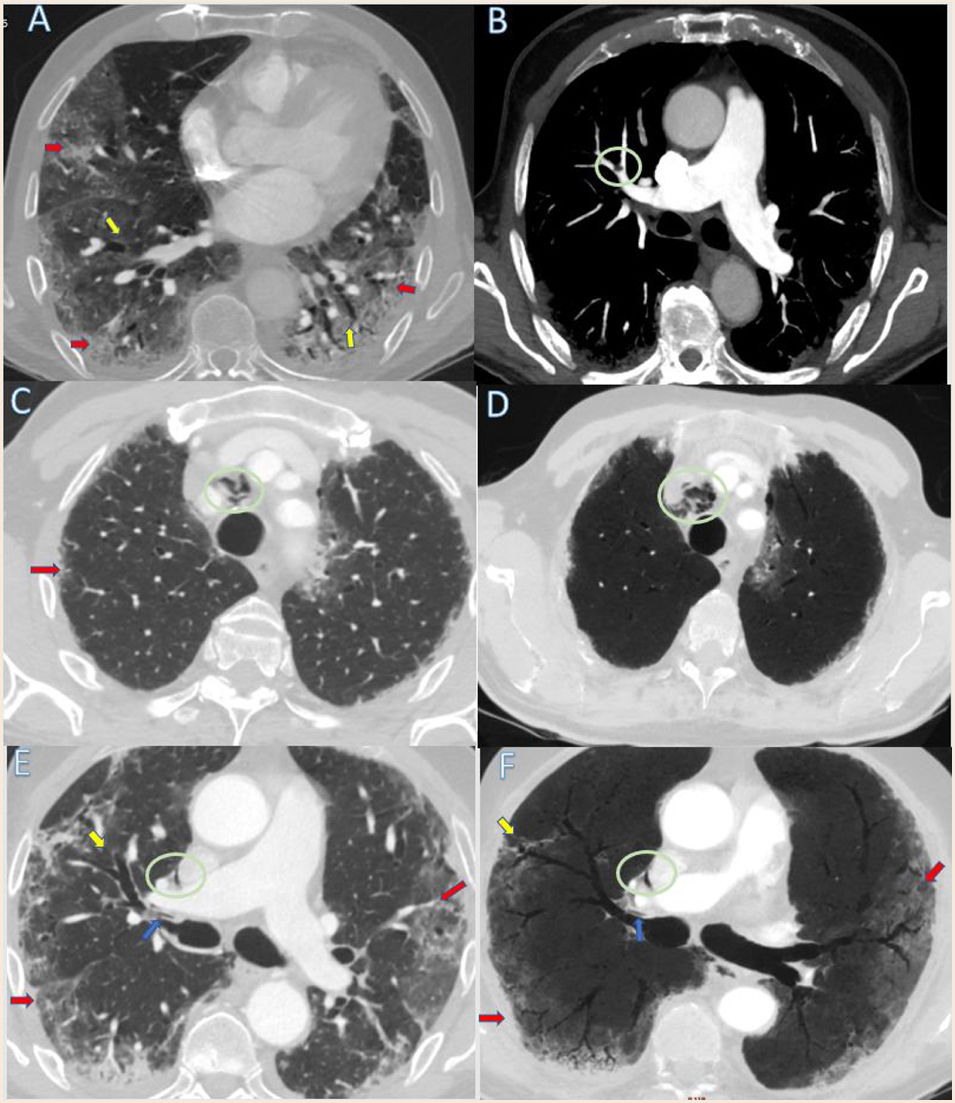
(A) Transverse CTPA images obtained with lung window setting shows multiple pulmonary parenchymal mainly peripheral ground glass opacities (red arrows). Bilateral varicose bronchiectasis (yellow arrows). (B) Maximum intensity projection (MIP) reconstructions images in axial plane shows filling defects (green circle) at the bifurcation level of the anterior segmental branch in right upper lobe compatible with pulmonary thromboembolism. (C–F) Transverse CT images with lung window (C and E) and reformatted Minimum intensity projection (MinIP) reconstructions (D and F) obtained at upper and medium mediastinic levels shows pulmonary interstitial emphysema with air tracking along the right peribronchovascular sheaths ((blue arrows). Central upper anterior right pneumomediastinum (green circles) secondary to a spontaneous barotrauma (Macklin effect). Multiple parenchymal ground glass opacities with prevalent peripheral distribution (red arrows). Bilateral varicose bronchiectasis (yellow arrows).
The patient was treated with anticoagulant therapy with progressive improvement of respiratory symptoms and decrease of D-Dimer values.
On day 19 of hospitalization the patient had a worsening of respiratory symptoms it was decided to practice a CTPA to exclude new PTE (D-Dimer 1050μg/L).
We detected a pulmonary interstitial emphysema, with air tracking along the right peribronchovascular with a central anterior right pneumomediastinum, that suggested pneumomediastinum secondary to a spontaneous barotrauma (Macklin effect) in a patient who was not intubated and who has not reported recent chest traumas (Fig. 1B–D, F).
Pneumomediastinum secondary to barotrauma (Macklin effect) is a very an unusual pulmonary complication to our knowledge, this is the first report about pneumomediastinum secondary to barotrauma with Macklin effect in a patient affected by Covid-19 pneumonia.1,2