Tracheopleural fistula is an extremely rare complication of chronic pulmonary tuberculosis as no similar case being published previously. A 52-year-old gentleman with history of chronic pulmonary tuberculosis (PTB) 20 years ago was presented with lethargy for 2 weeks associated with occasional haemoptysis. There was loss of weight and loss of appetite. No fever, shortness of breath, chest pain or night sweat. On examination, he was pale, afebrile, normotensive and not tachycardic. There was reduced air entry on the right lung with generalized coarse crepitations. Chest radiograph (Fig. 1a) showed right pneumothorax. Contrast-enhanced CT Thorax (Fig. 1b and c) confirmed presence of tracheopleural fistulae with thick-walled right pneumothorax. He was given intravenous (IV) tranexamic acid, blood transfusion and metered-dose inhaler (MDI) berodual and spiriva. He was stable under room air and discharged well after 5 days. He was planned for optimization of medical treatment as he refused surgical intervention or bronchoscopy. Chest tube was not done due to patient's refusal and clinically the oxygen saturation was acceptable. Tracheopleural fistula is rare and usually seen among cancer patients after chemotherapy.1 As opposed to tracheopleural fistula, tuberculous bronchopleural fistula is commonly seen although both conditions are rare.2 Clinical manifestations are varied among individuals and direction of treatment should be tailored individually to achieve good quality of life.
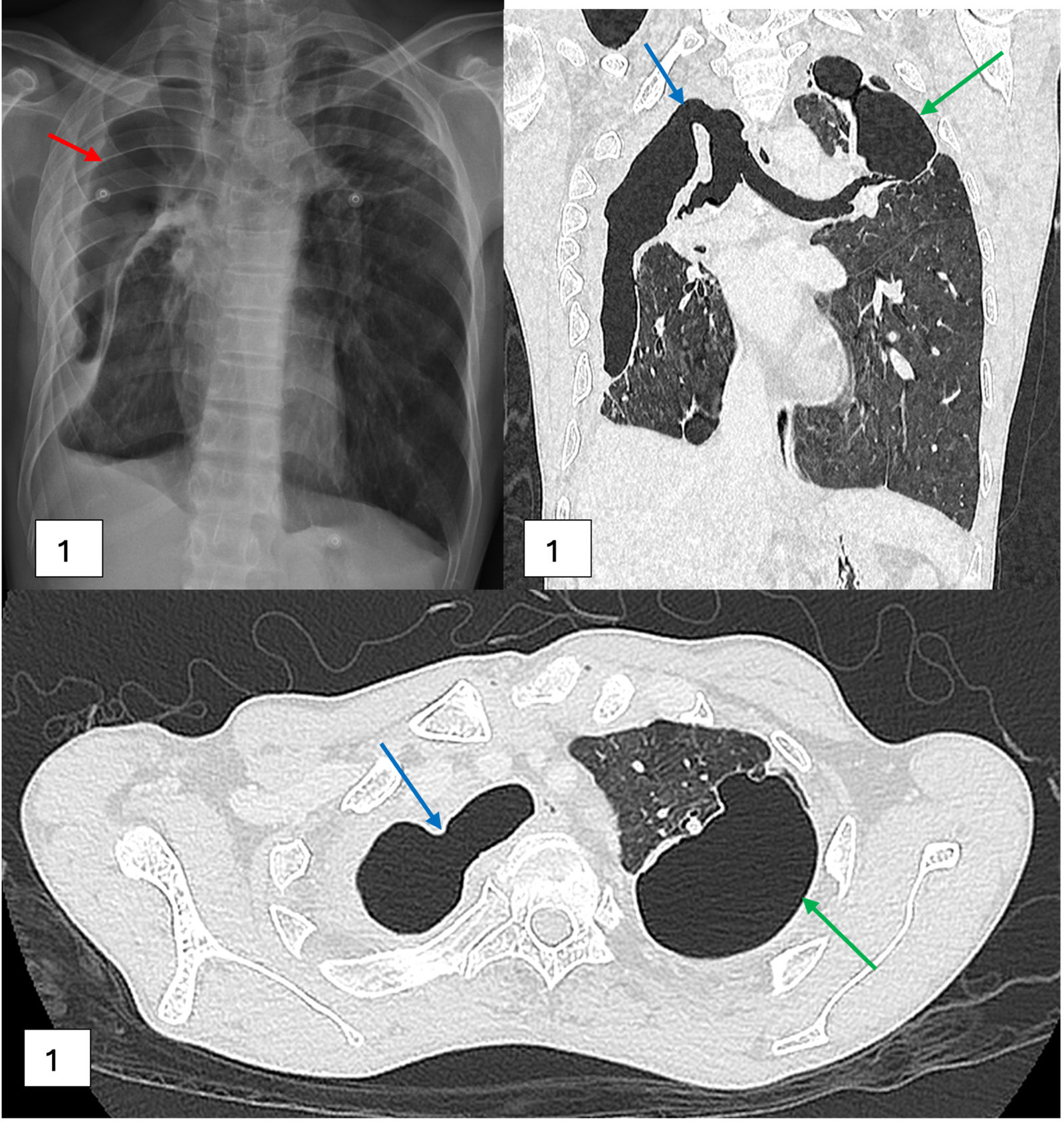
Chest radiograph showed right pneumothorax with pleural thickening (red arrow) (a). CECT Thorax in coronal (b) and axial (c) views revealed tracheal wall defects with direct communication with the pleural cavity, representing tracheopleural fistula (blue arrows). Left upper lobe lung bullae (green arrows) (b, c).
The authors state that they have no conflict of interests.