Primary thymic tumors are rare, but secondary ones are exceptionally uncommon. We report the case of a single metastasis within the thymic gland from a lung adenocarcinoma that had been completely resected 3 years before. There was high diagnostic doubt because the thymic lesion was not associated with the recurrence of the paraneoplastic syndrome or the increased CEA levels described at the moment of the treatment of the primary tumor. The lesion was diagnosed and treated at the same time by transcervical thymectomy. At the 1-year follow-up, the patient is alive and disease-free.
Los tumores primarios del timo son excepcionales, pero se han descrito unos pocos casos de tumores secundarios. Describimos el caso de una paciente con metástasis exclusivas en el timo a partir de un adenocarcinoma de pulmón resecado por completo 3 a¿nos antes. La duda diagnóstica aumentó porque la lesión tímica no se asociaba a la recidiva del síndrome paraneoplásico y a un aumento de los valores de antígeno carcinoembrionario (ACE) documentados en el momento del tratamiento del tumor primario. La lesión se diagnosticó y trató al mismo tiempo mediante timectomía transcervical. Al a¿no de seguimiento, la paciente sigue viva y libre de la enfermedad.
Primary tumors of the thymus are very rare, but secondary tumors have occasionally been described.1–3 In the clinical notes of the case that we present, we document an extremely rare case of exclusive metastasis in the thymus of a lung cancer that had been diagnosed and treated 3 years before.
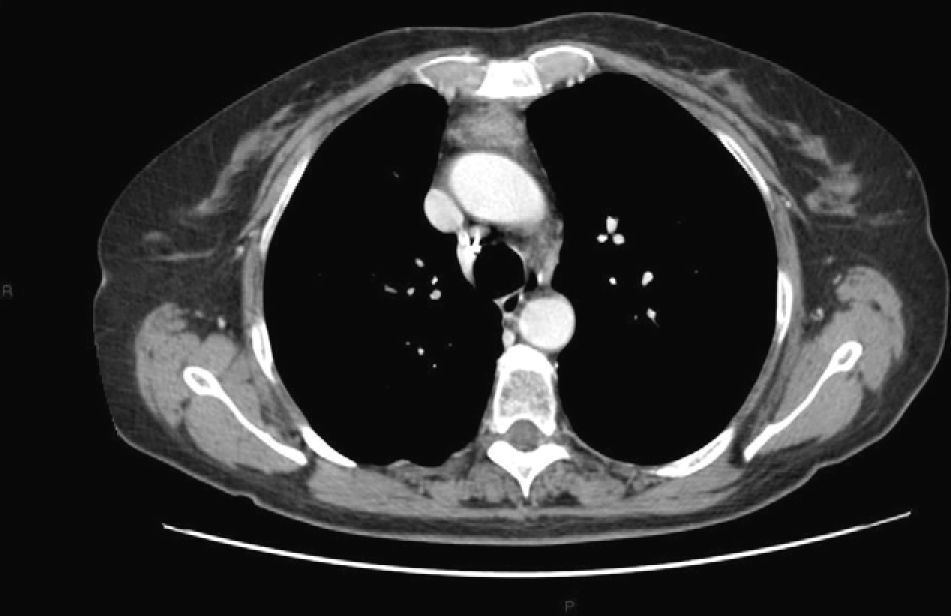
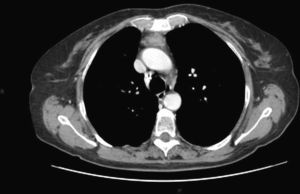
Case ReportIn May 2007, a 54-year-old woman with an important smoking history was referred to us due to an adenocarcinoma of the right lower lobe associated with a paraneoplastic syndrome (Pierre Marie Bamberg syndrome). At that time, she was found to have increased serum levels of carcinoembryonic antigen (CEA) (34ng/dl). Right lower lobectomy was carried out along with resection of the hilar and mediastinal lymph nodes by means of thoracotomy, which preserved the muscles of the right hemithorax. Three months after the surgery, we documented the complete regression of the paraneoplastic syndrome with the normalization of CEA serum levels (4ng/dl). The anatomic pathology evaluation of the samples confirmed a lung adenocarcinoma in stage pT2aN0. In the post-operative period, total body computed tomography (CT) was done every 6 months. In June 2009, a small solid lesion was found in the anterior mediastinum (max. diameter 1.8cm), while the serum levels of CEA continued to be normal and with the absence of paraneoplastic syndrome. In December 2009, CT revealed that the lesion in the anterior mediastinum had increased in size (max. diameter 3cm); with the administration of a contrast medium, the lesion was seen to be inhomogeneous, with a necrotic center (Fig. 1). No other intrathoracic or systemic lesions were seen. Serum CEA levels continued to be normal with absence of paraneoplastic syndrome. Positron emission tomography (PET)–CT demonstrated a lesion with the uptake of 18F-fluorodeoxyglucose-avid (maximal standardized uptake value 6.2). A thymic tumor was suspected, and thymectomy with en bloc resection of the tumor was carried out by means of cervicotomy and resection of the sternal manubrium.
The anatomic pathology testing of the sample suggested intrathymic metastasis of lung adenocarcinoma, which was confirmed by immunohistochemistry that was positive for TTF1 and CK7 stain and negative for CK20 and CK5 stain. Adjuvant chemotherapy was administered with platinum derivatives. After 1 year of follow-up, the patient was still alive and disease-free.
ConclusionsIt is known that, after surgical resection, lung cancer frequently recurs in the lymph node stations of the mediastinum and even the retrosternal region. In general, recurrent intrathoracic disease is also associated with systemic dissemination. It is likely that the lack of articles published about thymic metastasis of lung cancer is due to several reasons. In some cases, recurrent disease in the anterior mediastinum may be misinterpreted as a recurrence in the lymph nodes of the perivascular compartment instead of in the thymus; in other cases, thymic lesions are associated with other multiple systemic metastases in a situation of disseminated disease. For these reasons, both cases are considered to be of “limited” interest and they are either not cited or published. Thus, the true incidence of secondary thymic tumors may be underestimated.
Exclusive metastases of a carcinoma in the thymus are very rare. An autopsical series published in 1966 demonstrated a rate of 7% of isolated metastasis in the thymus from a carcinoma, while the incidence of isolated metastasis of a lung carcinoma was 1/18 cases (5%).4 Recently, Demondion et al.5 published a case of isolated metastases in the thymus from a lung adenocarcinoma that presented 3 years after the resection of the primary tumor. The diagnosis of recurrent disease in the thymus was confirmed after the surgical resection of the gland by sternotomy.
In the case described, the pre-operative clinical and radiological data were not clearly indicative of a primary or metastatic tumor. The data from the CT and PET–CT, such as the duplication time, appearance after the perfusion of the contrast medium and the maximal standardized uptake value (SUV) were more indicative of a metastatic lesion. On the other hand, the presence of an isolated mass, the absence of recurrence of the paraneoplastic syndrome and the persistence of normal serum levels of CEA during the follow-up of previous lung cancer were more indicative of a primary thymic tumor.
However, regardless of whether the patient were the carrier of either a primary or secondary thymic tumor, and taking into account the fact that the lesion was isolated, we made the decision to surgically resect the thymus that contained the undiagnosed lesion with both a diagnostic as well as a therapeutic objective.
Please cite this article as: Rena O, et al. Metástasis exclusivas en el timo de un cáncer de pulmón no microcítico resecado. Arch Bronco-neumol. 2012;48:423-4.