To estimate the cumulative incidence of COVID-19 and its determinants among a nationally representative sample of adults from Spain who smoke.
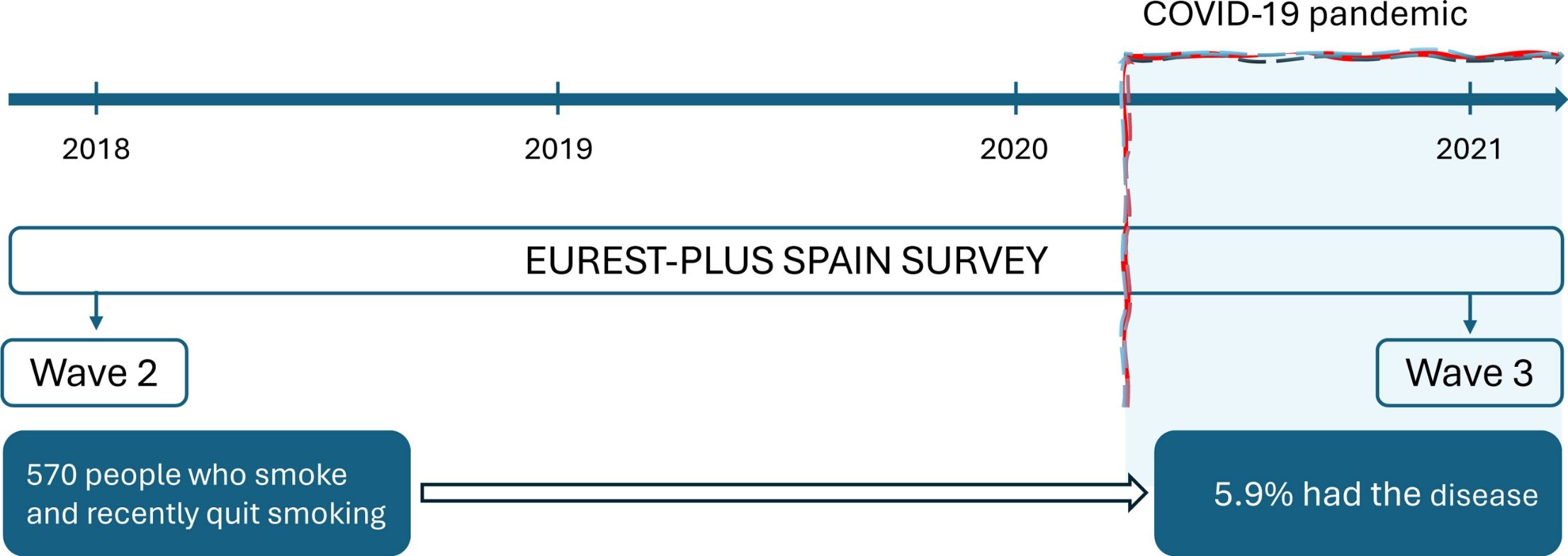
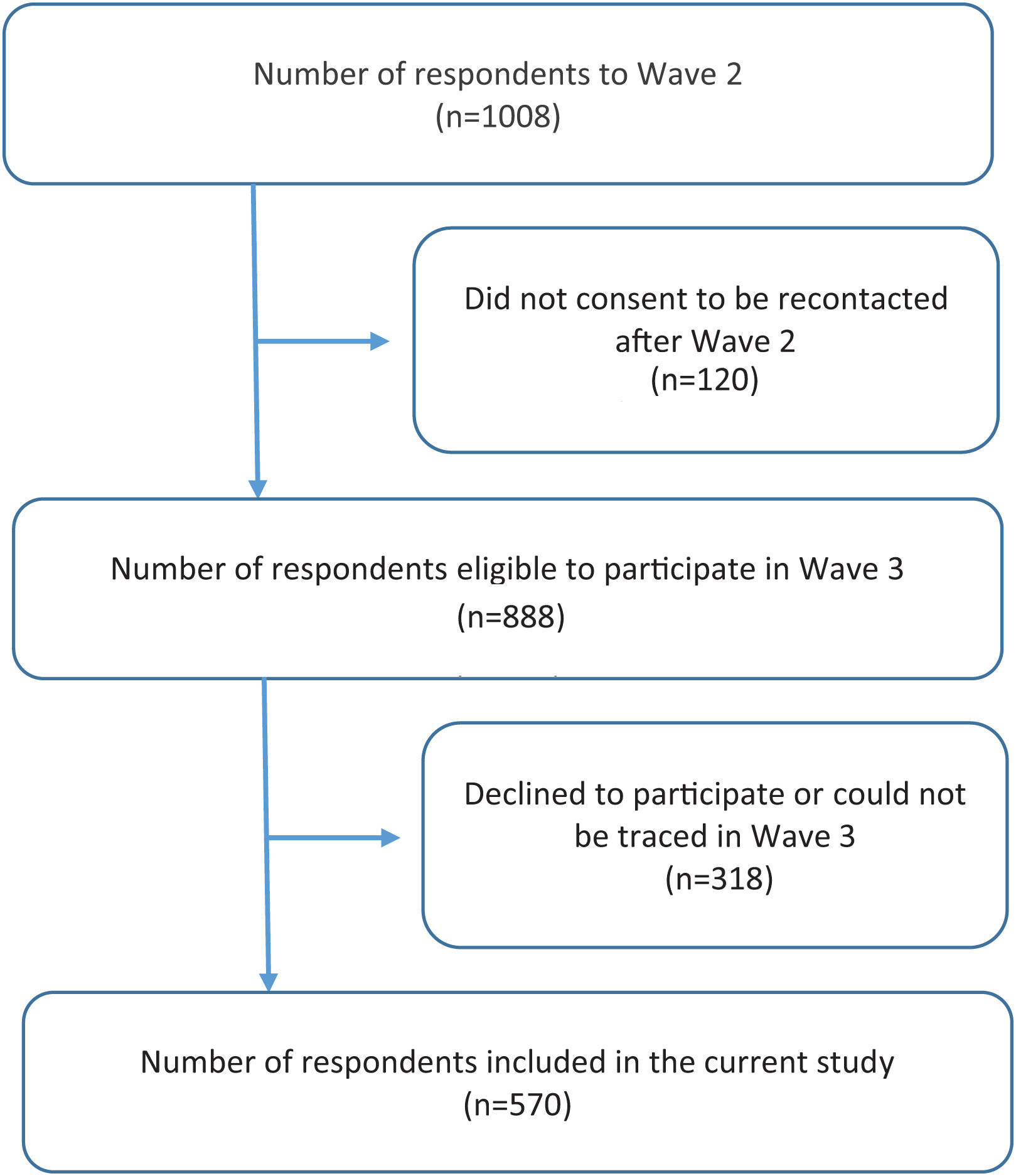
MethodsThis is a prospective cohort study that uses data from two waves (Wave 2 in 2018 and Wave 3 in 2021) of the ITC EUREST-PLUS Spain Survey. At baseline (Wave 1 in 2016), all respondents were adults (aged ≥18) who smoked. In total, 1008 respondents participated in Wave 2, and 570 out of 888 eligible participants were followed up in Wave 3 (64.2%). We estimated the cumulative incidence and the relative risk of COVID-19 (RR) and 95% confidence intervals (CI) during follow-up using self-reported information on sociodemographic, smoking-related and health-related characteristics and identified associated factors using multivariable Poisson models with robust variance adjusted for the independent variables.
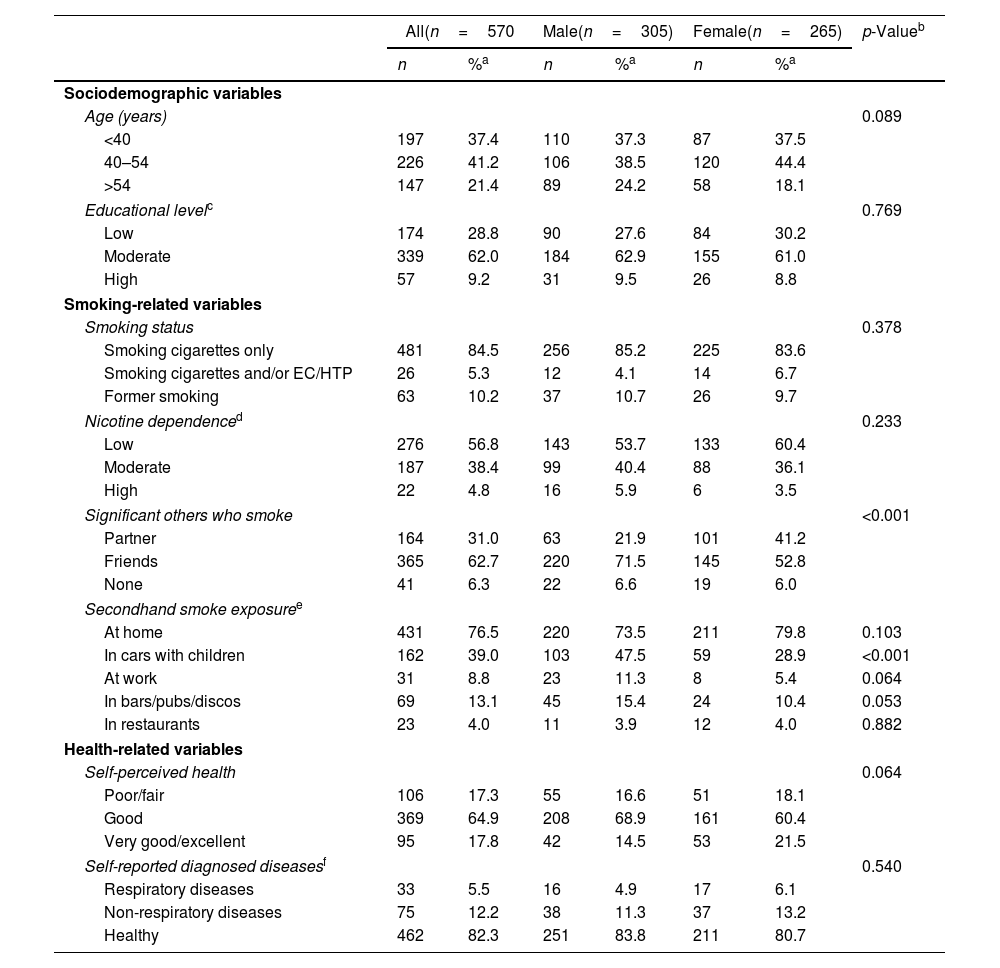
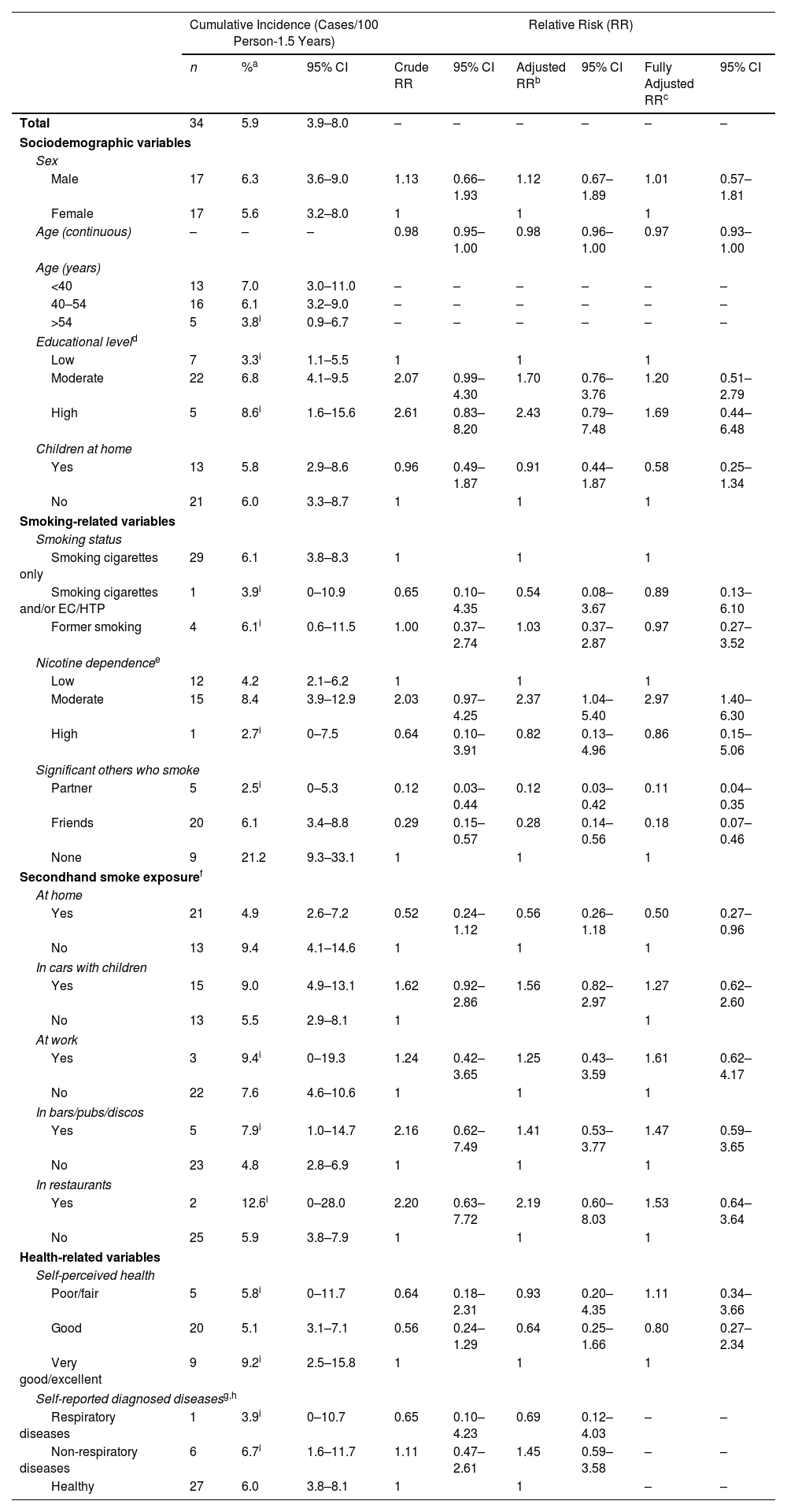
ResultsThe overall cumulative incidence of self-reported COVID-19 was 5.9% (95% CI: 3.9–8.0%), with no significant differences between males (6.3%; 95% CI: 3.6–9.0%) and females (5.6%; 95% CI: 3.2–8.0%). After adjusting for age, sex, and educational level, COVID-19 incidence was positively associated with moderate nicotine dependence (RR: 2.37; 95% CI: 1.04–5.40) and negatively associated with having a partner who smoked (RR: 0.12; 95% CI: 0.03–0.42), and having friends but not a partner who smoked (RR: 0.28; 95% CI: 0.14–0.56).
ConclusionThe correlates of having had COVID-19 among people who smoke should be considered when tailoring information and targeted non-pharmacological preventive measures.