Introduction
Flexible bronchoscopy was introduced by Ikeda in 1968.1 Its use in pediatric medicine, popularized by Wood and Fink,2 has increased steadily since the introduction in 1978 of the pediatric flexible bronchoscope with suction channel. The efficacy of flexible bronchoscopy as a diagnostic and therapeutic tool in pediatric practice has been demonstrated.3-5 It can, however, give rise to complications which the bronchoscopist should consider before carrying out the procedure, in order to draw up a risk-benefit analysis and determine whether bronchoscopy is justified.
Complications arising from bronchoscopy can be related to a number of factors: the bronchoscopic examination itself; factors relating to the patient, such as age or the severity of the illness; the sedation technique used to facilitate the procedure; and the skill, diligence, and experience of the bronchoscopist.6-10 In general, complications can be classified as mechanical, physiological, or infectious. Mechanical complications include airway trauma and obstruction, epistaxis, bronchial hemorrhage and perforation, and/or hemorrhage of the tracheal and bronchial mucosae.11,12 Physiological complications, which are caused by alterations in gas exchange or vagal tone, include hypoxemia, hypercapnia, bradycardia, cardiac arrhythmias, laryngospasm, bronchospasm, intense cough, hypotension, seizures, and even an increase in intracranial pressure.8,9,13 Infectious complications may affect both the patient and the medical personnel, so that all equipment should be sterilized between procedures, and appropriate techniques should be used to protect patients and staff.14 However, the incidence of serious complications attributable to bronchoscopy in pediatric patients is small.5,10,15 Most of the complications that occur are slight and transitory, and their frequency has been reported to be 2.9% to 3.1% of the procedures carried out.16,17 Depending on the way complications are defined and the pathology of the patients undergoing the procedure, however, some centers report a higher complication rate; incidences of over 10%,3 28%,18 and as high as 48%19 have been published. The few studies carried out to determine the factors associated with the presence of these complications concluded that patients with positive cultures in bronchoalveolar lavage (BAL), abnormal bronchoscopic findings, pathology of the upper airway, persistent radiographic abnormalities, dependence on supplemental oxygen, age under 2 years, and weight of under 10 kg are at higher risk of developing complications as a result of bronchoscopy.18,19
The object of this study was to determine the incidence of postbronchoscopy complications in pediatric patients and to identify the factors associated with such complications.
Material and Method
A retrospective cohort study was carried out in the Fundación Neumológica Colombiana-Fundación Cardioinfantil, a tertiary level clinic in Colombia specialized in pediatric respiratory diseases.
Pediatric patients between 1 month and 16 years old who had undergone bronchoscopy between January 1 and December 31, 2002 were identified from the foundation's records. In our institution, all bronchoscopic procedures in pediatric patients are performed under general anesthesia in the operating room because of the better control of the airway this affords and the ease of monitoring and caring for the patient in this environment.
The medical team in charge of performing bronchoscopies always includes a duly certified pediatric pulmonologist with 5 years of experience in performing pediatric bronchoscopies. In addition, all bronchoscopic procedures are attended by a doctor specialized in anesthesiology with experience in the airway management of pediatric patients and by a nurse in charge of monitoring the patient and administering the necessary medication.
Written informed consent is obtained prior to all bronchoscopies. The procedures are carried out in accordance with the guidelines drawn up by the American Academy of Pediatrics and the American Thoracic Society for the monitoring and performance of bronchoscopies in pediatric patients.20 Patients receive no food or fluids by mouth for at least 6 hours before the procedure, and intravenous access is established in a peripheral vein.
The choice of anesthetic and the dose used is determined by the anesthesiologist in accordance with his or her experience and the patient's age, underlying disease, and physiological state. When considered necessary, a dose of atropine is administered to reduce bronchial secretions.
The procedure is performed using an Olympus pediatric bronchoscope (Olympus America; Melville, NY, USA) with an outer diameter of 3.6 mm, and/or a rigid bronchoscope with an outer diameter between 3.7 mm and 8.2 mm (depending on the age of the patient) when foreign bodies are being extracted. BALs are performed with aliquots of 0.9% NaCl once the bronchoscope is properly positioned. The total amount of 0.9% NaCl for lavage does not exceed 3 mL/kg. The procedure is terminated early if, in the opinion of the pediatric pulmonologist and the anesthesiologist, there are severe desaturations that do not readily respond to removing the bronchoscope, manipulating the airway, or increasing inspired oxygen concentration. Similarly, in the event of deterioration in the patient's clinical status, if a complication develops, or if they consider that the patient requires closer monitoring, the pediatric pulmonologist and the anesthesiologist decide whether the patient should be transferred to the intensive care unit (ICU). If this is not necessary, after the procedure has been performed, the patient is transferred to the recovery room, where he or she remains until completely awake and capable of ingesting liquids without risk of aspiration.
In order to determine whether or not complications had developed, 2 pediatric residents reviewed the clinical records, anesthesia reports and postbronchoscopy nursing notes for all the cases studied. All complications identified were then recorded on a database designed for this purpose.
In this study, we defined complications as events or conditions we considered could have compromised the patient's condition or put his or her life in danger21 during the procedure and/or during the first 24 hours postprocedure. Complications analyzed were desaturation (defined as a fall of 10% or more from baseline), presence of or increase in coughing, bronchial obstruction, stridor, retractions, fever, laryngospasm, upper airway obstruction, apnea, bradycardia, epistaxis, arterial hypotension, vomiting, and death. Transfer to the ICU was also considered a complication. In spite of the fact that the relationship between oxygen pressure and the percentage of hemoglobin saturation is not linear,22 we defined desaturation to be a complication when there was a fall of 10% or more from baseline. We did this to facilitate the definition and analysis of the event and to enable comparison with other studies, given that other authors have used this definition.18
The predictive variables were as follows: age; sex; medication used for sedation or anesthesia (halothane, midazolam, or ketamine); type of airway access used (laryngeal mask, endotracheal tube, or facial mask); use of atropine prior to the procedure (yes or no); need for supplemental oxygen before the bronchoscopy or oxygen saturation of less than 90% breathing room air as monitored by pulse oximetry before the procedure (yes or no); performance of BAL (yes or no); duration of the procedure determined using anesthesia records (<30 min or >30 min); bacterial growth in BAL (yes or no); and the use of a rigid bronchoscope in addition to a flexible bronchoscope (yes or no).
Statistical analysis was carried out using the SPSS statistical software package version 10.0 (Chicago, Illinois, USA). Continuous variables are shown as means (SD). Differences between categorical variables with respect to the presence or absence of complications were analyzed using the χ² test or Fisher exact test, whichever was appropriate. A logistic regression model was devised to estimate the crude and adjusted odds ratios (OR) identifying independent risk factors associated with the presence of complications. Predictive variables significantly associated with outcome variables in the bivariate analysis were included in the multivariate analysis. The magnitude of the effect of each of the risk factors was measured using the OR and their 95% confidence interval (CI). All statistical tests were 2-tailed, and the significance level used was .05.
Results
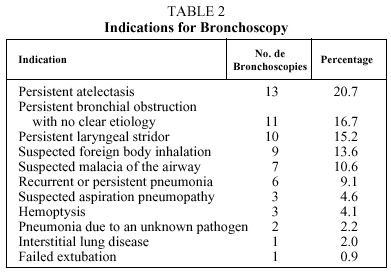
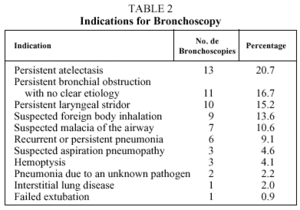
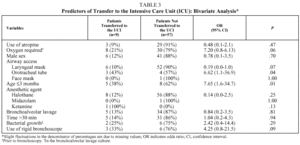
During the period studied, 66 bronchoscopies were performed; in 61 (92%) only a flexible bronchoscope was used, and in 5 (8%) both flexible and rigid bronchoscopes were used. A rigid bronchoscope was used when a foreign body was detected in the airway. Of the 66 patients, 7 (10.6%) were on conventional mechanical ventilation at the time the procedure was performed. Of the total number of patients, 47 (71%) were males and the remaining 19 (29%) females. The median (interquartile range) age was 9.5 (4.75-27.75) months. Of the 66 procedures, 56.1% were performed in patients less than 1 year old, 21.2% in patients between 1 and 3 years old, and 22.7% in children more than 3 years old. The mean duration of the bronchoscopies was 43.1 (22.2) minutes. Table 1 shows the frequencies of the other predictive variables among the patients included in the study. The indications for performing bronchoscopy are shown in Table 2. The evaluation of the airway was abnormal in 68.1% of the procedures, and the performance of bronchoscopy contributed significantly to treatment in 65.1% of patients, especially in those in whom the procedure was performed because of suspected foreign body aspiration (88.8%), persistent laryngeal stridor (80%) and suspected malacia of the airway (71.4%). BAL was abnormal in 76.9% of the 39 carried out, but these results contributed little to subsequent treatment, except in patients with suspected aspiration pneumopathy (66.6%). Bacteria grew in 20.5% of the 39 lavage cultures, but these findings only led to modification of treatment in very few cases. Airway evaluation, BAL, and the result of the BAL culture together contributed to the patient's treatment in 53 cases (80.3%).
Of the 66 patients, 22 (33.3%) developed some kind of complication, and 10 (15.2%) presented important complications (apnea, laryngospasm, and/or transfer to ICU). The most frequently occurring complications were desaturation of 10% or more with respect to the baseline value in 18 patients (27.3%), the need for transfer to the ICU in 9 patients (13.6%), and an increase in coughing after the procedure in 4 patients (6.1%). In 4 (22.2%) of the 18 patients who presented desaturation of 10% or more, it was necessary to terminate the procedure prematurely. No patient presented with epistaxis, vomiting, or bradycardia; and none of the patients died as a direct result of the bronchoscopy.
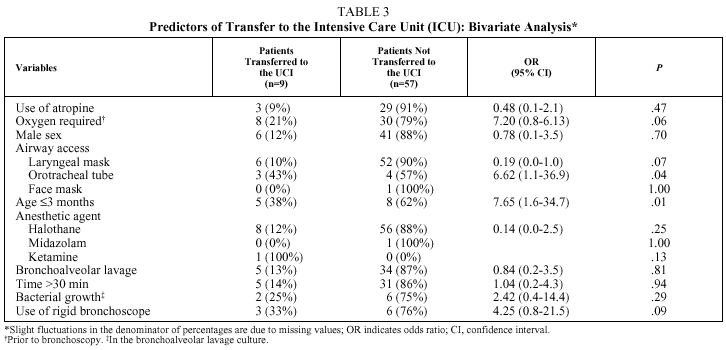
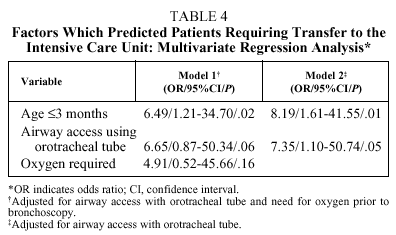
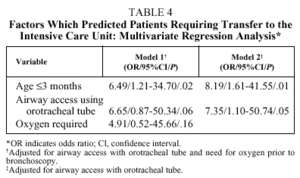
The only complication considered independently associated with any of the predictive variables was the need for transfer to the ICU, which was significantly related to the use of an orotracheal tube to access the airway (OR=6.62; 95% CI, 1.18-36.94; P=.04) and with patient age of 3 months or less (OR=7.65; 95% CI, 1.68-34.74; P=.01) (Table 3). However, in the multivariate analysis, after adjusting for airway access with orotracheal tube, patient age of 3 months or less was the only independent factor associated with the need for transfer to the ICU (model 2, Table 4). This result did not change to any relevant degree when dependence on supplementary oxygen before bronchoscopy--a variable almost associated in the bivariate analysis (model 1, Table 4)--was included in the multivariate analysis.
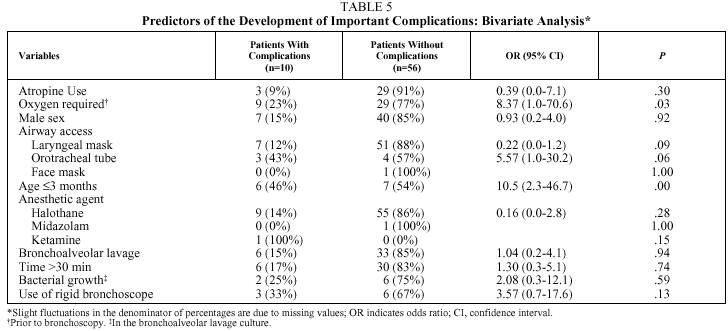
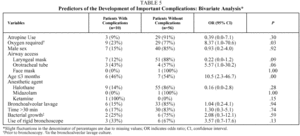
Table 5 shows the predictors of important complications in the bivariate analysis. No statistically significant differences were found between patients with or without important complications in the use of atropine before bronchoscopy, the sex of the patient, the type of airway access used, the anesthesia medication used, or the indication for which the bronchoscopy was performed. Patient age of 3 months or younger (OR=10.50; 95% CI, 2.36-46.71; P=.003) and need for supplemental oxygen before the procedure (OR=8.37; 95% CI, 1.05-70.61; P=.03) were significantly associated with the presence of important complications.
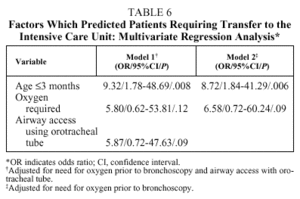
Predictive variables significantly associated with outcome variables in the bivariate analysis were included in the multivariate analysis. After adjusting for the effect of supplemental oxygen before bronchoscopy, we found that patient age of 3 months or younger was the only independent factor associated with the presence of important complications (model 2, Table 6). This result did not change to any relevant degree when the model included airway access using an orotracheal tube--a variable almost significantly associated in the bivariate analysis (model 1, Table 6).
Discussion
Although until recently the role of fiberoptic bronchoscopy in the field of pediatric medicine was considered uncertain, today this technique is seen as an important and useful tool in the diagnosis and treatment of a wide variety of pediatric respiratory pathologies.2,9 However, the procedure can give rise to complications, most of which are slight and transitory.3 Of the 66 patients included in our study, 22 (33.3%) developed some kind of complication, the 2 most common being desaturation of 10% or more with respect to baseline values and the need for transfer to the ICU. No patients experienced epistaxis, vomiting, or bradycardia; and none of them died as a direct consequence of the bronchoscopy. The incidence of complications found in this study is higher than that reported in some units,3,16 similar to that found in others,18 and lower than that reported in others.19 This difference may be attributable to various factors including the way complications are defined, when they are evaluated, factors related to the patients (such as age, underlying disease, and the severity of the respiratory disease), and to the type of sedation or anesthesia used. Of the 66 patients in this study, 10 (15.2%) developed complications that were considered important (apnea, laryngospasm, and/or need for transfer to the ICU) during and/or after the procedure; however, none of the patients died as a direct consequence of a bronchoscopy. This result is consistent with the safety and absence of mortality associated with the procedure reported in the literature.11,17
On determining the factors associated with the presence of complications, we found that, after adjusting for airway access using an orotracheal tube, patient age of 3 months or less was the only independent factor associated with the need for transfer to the ICU. Moreover, after adjusting for the effect of requiring supplemental oxygen before bronchoscopy, we found that age of 3 months or less was the only independent factor associated with the presence of important complications. This greater probability among younger patients of developing complications has been reported by other authors, who have found that patients under 2 years old19 and those weighing less than 10 kg18 have a higher risk of developing complications postbronchoscopy. Younger patients may be at higher risk of developing complications for various reasons. In the first place, because the bronchoscope at least partially obstructs the airway, it can generate abnormally high pressure gradients and considerable change in airway dynamics, which may lead to collapse of the peripheral airways. This effect is much more marked in younger patients because of the smaller diameter of their airways. This means that the bronchoscope occupies a larger proportion of the lumen, making it more likely that its passage will provoke collapse of the peripheral airways, whose structure does not yet provide sufficient support. Moreover, the greater distensibility of the thoracic cage in younger patients makes it impossible to create sufficient intrapleural negative pressure to sufficiently expand the lungs, in turn preventing the infant's thorax from achieving its ideal volume, thereby facilitating airway collapse. Moreover, in young infants this greater distensibility of the thoracic cage means that continuous tone of the inspiratory muscles of the thorax is particularly important in the maintenance of functional residual capacity, which tends to decrease owing to the lack of rigidity of the thoracic cage needed to oppose the elastic recoil of the lung.20 General anesthesia, which was used in the majority of our patients, attenuates or suppresses this inspiratory muscle activity, thereby further reducing the expansive force of the thorax and the functional residual capacity.23 This decrease in functional residual capacity, the consequent collapse of the airway, and the decrease in hypoxic pulmonary vasoconstriction produced by general anesthetics are the factors responsible for the alteration in the distribution of ventilation and perfusion, which causes an increase in the venous admixture.24
An additional fact that may explain why a higher incidence of complications has been observed in very young children is their greater susceptibility to airway obstruction after the administration of a general anesthetic because the muscles of the upper airway in infants are more sensitive to the depressant effects of the general anesthetic than those of older children and adults.25
One source of bias in this study is that the person who decided whether or not the patients had developed complications knew whether or not they had been exposed to a specific predictive variable. This person was not, however, aware of the study hypothesis, and the data was collected in the most standarized and objective way possible.
On the basis of our findings, we recommend that when a decision is being taken on whether or not to use bronchoscopy in a patient aged under 3 months, a rigorous analysis of the benefits of the procedure and the possible complications it might cause should be carried out. Although these complications are not usually serious, in some cases they require monitoring and management in the ICU. Furthermore, our opinion is that the use of sedation rather than a general anesthetic for this procedure should be considered in order to avoid the effects of general anesthesia on respiratory mechanics and thereby reduce the complication rate. This is already common practice in many centers.
Acknowledgments
We would like to thank the pediatric residents María Elvira Sarta and Claudia Camacho for their invaluable help in collecting and recording information, and Dr Guillermo Ortiz and Dr Ricardo Aristizábal for their collaboration in the revision of the manuscript.
Correspondence: Dr. C. Rodríguez Martínez.
Fundación Neumológica Colombiana. Fundación Cardioinfantil.
Calle 163, A, 28-60. Bogotá. Colombia.
E-mail: carlos2671@hotmail.com
Manuscript received March 27, 2003.
Accepted for publication June 3, 2003.