Obstructive sleep apnea (OSA) is the most prevalent type of sleep-disordered breathing which has increasingly caused multiple health problems, particularly in the last decades due to the worsening of the obesity epidemic.1 OSA has repeatedly been associated with a number of cardiovascular conditions and is thus considered a potential risk factor for cardiovascular disease.2 Furthermore, treatment with continuous positive airway pressure (CPAP) has been shown to reduce cardiovascular disease burden in large observational studies.3
Nevertheless, a recent randomised controlled trial (RCT) failed to demonstrate that treatment of OSA, by means of continuous positive airway pressure (CPAP), is associated with a reduction of cardiovascular events and mortality.4
These results were somehow unexpected, as CPAP is known to mitigate sympathetic activation caused by OSA, and to reduce, not only awake blood pressure (BP), but also the BP swings due to the intermittent apneic and hypopneic cycles, one of the hallmarks of the disease.5,6
A number of possible explanations for this finding have been proposed.
Adherence to CPAP is often suboptimal in RCTs, as was the case in the largest RCT in the field, where average duration of nightly CPAP usage was 3.3h.4 This is below what is commonly considered to be the minimum average daily usage that favours a beneficial treatment effect and is below the threshold for coverage of PAP devices by many third party payers.7,8 However, there was no significant effect on cardiovascular events even in the more adherent CPAP users.4
In addition to this, CPAP treatment can sometimes disturb the patient's sleep by causing awakenings, particularly if the air pressure titration is not conducted appropriately: studies have shown that excessively high CPAP pressures can not only lead to increased neural respiratory drive and subjective discomfort while awake, but can also cause rises in BP and contribute to increased BP variability.9,10
Conversely, setting sub-therapeutic CPAP pressures may fail to abolish apneas and hypopneas, thus leaving the patient under-treated and with residual OSA.
Finally, patient selection may be another limitation, with many RCTs excluding highly symptomatic or sleepy patients who may be more likely to adhere to CPAP. Additionally, patients with excessive daytime sleepiness are more likely to have hypertension, metabolic dysfunction, and cardiovascular morbidity compared to those without.3
With regard to the effect of CPAP on cardiovascular outcomes, BP has often been studied as a surrogate marker for cardiovascular risk for several reasons: it is relatively easy to measure, it is cost effective, and it is widely available. Most importantly, in other situations, BP is linearly associated with the risk of cardiovascular events and many studies have shown that OSA treatment results in a modest but significant BP reduction.11
All studies looking at the effects of CPAP on BP have shown a large interindividual variation in the response, with some subjects experiencing rises in BP rather than falls. A recent systematic review and meta-analysis on the BP effects of OSA treatment, mostly focusing on CPAP use, showed that some subgroups of patients exhibited a greater BP response to treatment, i.e. those who were younger (aged<60 years), with uncontrolled BP at baseline and with severe oxygen desaturations were more likely to benefit from treatment.12 It is important to note that such variables were not available in all RCTs highlighting the need for a thorough patient characterisation prior to initiating OSA treatment.
Such aggregate data meta-analysis can help to detect specific subgroups and phenotypes which respond better to OSA treatment. Data obtained in this manner, however, might suffer from limitations such as publication bias, heterogeneity between the various study designs, model selections, different analysis approaches, and variable categorisations of the original studies.
One way to reduce such limitations is to conduct an individual patient data (IPD) meta-analysis which is considered the “gold standard” for exploring the effectiveness of a given intervention in different patient cohorts.13
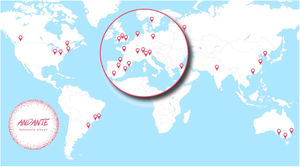
It was indeed with the aim to run an IPD meta-analysis in patients with OSA that the ANDANTE (effect of treatment for obstructive sleep apnea on blood pressure: an individual patient data meta-analysis) project was conceived and implemented, by building a worldwide collaboration among the principal investigators of most available RCTs on BP effects of OSA treatment (Fig. 1). These researchers were invited to share the individual data of their previously published RCTs in order to merge them in a single database, thereby allowing for a refined meta-analysis with sensitivity analyses on a large scale, to better understand predictors of BP response in different patient groups.
The primary objective of the ANDANTE collaboration is to confirm the results of our previously published meta-analysis of aggregate data.12 The secondary objective is to refine the cutoffs for age, BP at baseline and oxygen saturation at which OSA treatment achieves the best BP reduction. Tertiary objectives are to explore other predictors of BP reduction with OSA treatment and to separately investigate changes in 24h, daytime and nighttime BP, as well as in nocturnal BP dipping and in BP variability indices induced by OSA treatment.
Potential limitations of such an approach to explore the BP effects of OSA treatment include the number of RCTs where the individual data are no longer available, thus preventing their inclusion in the meta-analysis, and the relative paucity of studies investigating the role of non-CPAP therapies on BP.
Nevertheless, the ANDANTE project will include data from more than 60% of the available studies (see list of Andante investigators in the acknowledgments), thus likely enabling us to satisfactorily characterise patient phenotypes associated with greater or smaller BP reduction. Another important point to be addressed is the characteristics of patients who are likely to benefit from OSA treatment in preventing cardiovascular diseases. Interestingly, in the Sleep Apnea Cardiovascular Endpoints (SAVE) trial the mean age of the included subjects was 61.3 years and the mean BP was within normal limits at baseline (131/79mmHg).4 In our previously published meta-analysis, this phenotype was associated with a reduced BP response whilst on CPAP treatment and this might, at least in part, explain the negative results on the primary outcome of the trial. The ANDANTE study is designed to further clarify this issue by allowing us to consider individual data and thus to identify possible confounders of the protective effect of OSA treatment vs cardiovascular outcome on an individual basis.
We thus expect the ANDANTE collaboration to shed some further light on predictors of greater BP reduction among OSA patients treated with CPAP. Despite the large number of RCTs conducted, current guidelines and recommendations support the treatment of OSA with the aim of reducing BP, but do not define clear BP thresholds nor identify phenotypes of hypertensive patients in whom this approach could be most useful and successful, or indeed potentially harmful.14
The task force of the American Academy of Sleep Medicine (AASM) suggested in their clinical practice guidelines to use positive airway pressure (PAP) therapy to treat OSA in adult patients with co-morbid hypertension, but again, without defining specific BP cut-offs.15
The task force noted that the overall quality of evidence, based on the critical outcome of mean arterial BP, was moderate due to imprecision. They concluded that in adult patients with OSA and co-morbid hypertension, the benefits of CPAP therapy compared to no CPAP therapy likely outweighed its potential harms and burdens, and that the majority of well-informed patients would choose the intervention over no treatment.15
This view is understandable however, there remain various views as to whether asymptomatic patients with hypertension would accept CPAP. We believe that the field of sleep-disordered breathing is now in the position to endorse a precision medicine approach. On one side this will avoid over-delivery of treatment in asymptomatic patients with OSA, with the sole aim of preventing possible cardiovascular complications. On the other side it will avoid OSA treatment in those patients with individual features requiring a therapeutic intervention and associated with the possibility of greater BP reduction with treatment. In the latter case, a personalised approach will also be particularly useful to tailor optimal therapeutic options in individual patients and to improve their adherence to CPAP treatment as much as possible.
To conclude, in the present and future era of precision medicine, collaboration of all actors involved in healthcare delivery is an essential requirement for the provision of best possible care, aimed at improving diagnostic criteria, primary and secondary prevention implementation, and treatment efficacy, based on a holistic, individually tailored approach.
The ANDANTE project will contribute to a greater precision in managing OSA by identifying individual predictors of BP response to treatment and by providing information about the effect of OSA treatment in the less studied patients’ phenotypes such as women and asymptomatic or non-obese patients. This will help clinicians identify patients who benefit the most from OSA treatment and provide individually tailored treatments that may better impact on cardiovascular outcomes. It will also provide valuable data on which to base future intervention trials that aim to demonstrate the benefit of OSA treatment on these same outcomes.
The authors gratefully acknowledge the support of the ANDANTE investigators, patients and collaborators. In particular, ANDANTE collaboration include the researchers (listed in alphabetical order, appendix).
The authors gratefully acknowledge the support of the ANDANTE investigators, patients and collaborators. In particular, ANDANTE collaboration include the following researchers (listed in alphabetical order): Najib T. Ayas (Department of Medicine, University of British Columbia, Vancouver, BC, Canada); Ferran Barbé (Centro de Investigación Biomédica en Red de Enfermedades Respiratorias (CIBERES), Madrid, Spain); Maree Barnes (Faculty of Medicine, Dentistry and Health Sciences, The University of Melbourne, Melbourne, Australia and Institute for Breathing and Sleep, Austin Hospital, Heidelberg, Australia); Francisco Campos-Rodriguez (Respiratory Dept, Hospital Universitario de Valme, Sevilla, Spain); Peter Cistulli (Charles Perkins Centre, University of Sydney, and Department of Respiratory & Sleep Medicine, Royal North Shore Hospital, St Leonards, NSW, Australia) Patricia Lloberes (Servei de Pneumologia, Hospital Vall Hebron, Barcelona, Spain, Centro de Investigación Biomédica en Red de Enfermedades Respiratorias (CIBERES)); Sonya Craig (Liverpool Sleep and Ventilation Centre, University Hospital Aintree, Liverpool, UK); Luciano F Drager (Heart Institute (InCor) University of São Paulo Medical School, Brazil, Hypertension Unit, São Paulo, Brazil); Joaquín Durán-Cantolla (Research Service and Bioaraba Research Institute, OSI Araba University Hospital, UPV/EHU, Vitoria, Spain); Alexander Litvin and Evgeniya Elfimova (Federal State Budgetary Institution, National Medical Research Center of Cardiology, Ministry of Health of the Russian Federation, Department of Hypertension, Moscow, Russian Federation); Tasali Esra (Department of Medicine University of Chicago IL, USA); Alice Giontella and Cristiano Fava (Department of Medicine, University of Verona, Italy); Sandra Costa Fuchs and Flávio Danni Fuchs (Division of Cardiology, Hospital de Clínicas de Porto Alegre, Porto Alegre, RS, Brazil); Frédéric Gagnadoux (Université Bretagne Loire, INSERM UMR, Angers, France); Francisco García-Río (Neumología, Hospital Universitario La Paz, Madrid, Spain); Sogol Javaheri and Daniel J Gottlieb (Brigham and Women's Hospital, Harvard Medical School, Boston, MA, USA); Geu-Ru Hong (Division of Cardiology, Severance Cardiovascular Hospital, Seoul, Republic of Korea); Ronald R Grunstein (Faculty of Medicine and Health, University of Sydney and, Centre for Sleep and Chronobiology, Woolcock Institute of Medical Research, University of Sydney, New South Wales, Australia); Camilla M Hoyos (School of Psychology, Brain and Mind Centre, University of Sydney and, Centre for Sleep and Chronobiology, Woolcock Institute of Medical Research, University of Sydney, New South Wales, Australia); Marie Joyeux-Faure (HP2 Laboratory, Inserm Unit 1300, University Grenoble Alpes and EFCR Laboratory, Grenoble Alpes University Hospital, Grenoble, France); Peter Y. Liu (The Lundquist Institute of Biomedical Innovation. Harbor-UCLA Medical Center, USA); Geraldo Lorenzi-Filho (leep Laboratory, Pulmonary Division, Heart Institute (InCor), Av. Enéas Carvalho de Aguiar, 44, São Paulo, Brazil); Mary S M Ip and Macy M S Lui (Division of Respiratory and Critical Care Medicine, Department of Medicine, Queen Mary Hospital, University of Hong Kong, Pokfulam, Hong Kong SAR, China); Miguel Ángel Martínez-García (Pneumology Department, Hospital Universitario and Politécnico La Fe, Valencia, Spain); Doug McEvoy (Adelaide Institute for Sleep Health (AISH) and the School of Medicine, College of Medicine & Public Health, Flinders University, and Sleep Health Service, Respiratory and Sleep Services, Southern Adelaide Local Health Network, Adelaide, Australia); Reena Mehra (Cleveland Clinic, Cleveland Ohio, USA); Carmen Monasterio ((Multidisciplinary Sleep Unit, Department of Respiratory Medicine, Hospital Universitari de Bellvitge, L’Hospitalet de Llobregat, Spain; Section of Respiratory Medicine, Bellvitge Biomedical Research Institute (IDIBELL), L’Hospitalet de Llobregat, Spain; Centro de Investigación Biomédica en Red de Enfermedades Respiratorias (CIBERES), Spain)); Alison McMillan and Mary J Morrell (Academic Unit of Sleep and Ventilation, National Heart and Lung Institute, Imperial College London, London, UK; Respiratory Disease Biomedical Research Unit at the Royal Brompton Hospital and Harefield NHS Foundation Trust, London, UK); SushmitaPamidi (Respiratory Division, Department of Medicine, McGill University, Montreal, Quebec, Canada); Martino Pengo, Grzegorz Bilo, Carolina Lombardi and Gianfranco Parati (Istituto Auxologico Italiano, IRCCS, Department of Cardiovascular, Neural and Metabolic Sciences, S.Luca Hospital, Milan, Italy; Department of Medicine and Surgery, University of Milan-Bicocca, Milan, Italy); Yüksel Peker (Koc University School of Medicine, Koc University Research Center for Translational Medicine (KUTTAM), Istanbul, Turkey); Martin Glos and Thomas Penzel (Center for Sleep Medicine, Charité—Universitätsmedizin Berlin, Berlin, Germany); Jean-Louis Pépin (HP2 Laboratory, Inserm Unit 1300, University Grenoble Alpes and EFCR Laboratory, Grenoble Alpes University Hospital, Grenoble, France); Justin C T Pepperell (Somerset Lung Centre, Musgrove Park Hospital, Taunton and Somerset NHS Foundation Trust, Taunton, United Kingdom); Craig L Phillips (Faculty of Medicine and Health, University of Sydney and, Centre for Sleep and Chronobiology, Woolcock Institute of Medical Research, University of Sydney, New South Wales, Australia); Stuart F Quan (Asthma and Airways Disease Research Center, University of Arizona, Tucson, AZ, USA); Tim Quinnell (Royal Papworth Hospital NHS Foundation Trust, Cambridge, UK); Gil F Salles (Department of Internal Medicine, School of Medicine, Universidade Federal do Rio de Janeiro, Rio de Janeiro, Brazil); Neus Salord (Multidisciplinary Sleep Unit, Department of Respiratory Medicine, Hospital Universitari de Bellvitge, L’Hospitalet de Llobregat, Spain; Section of Respiratory Medicine, Bellvitge Biomedical Research Institute (IDIBELL), L’Hospitalet de Llobregat, Spain; Centro de Investigación Biomédica en Red de Enfermedades Respiratorias (CIBERES), Spain); Manuel Sánchez-de-la-Torre (Group of Precision Medicine in Chronic Diseases, Hospital Arnau de Vilanova and Santa Maria, IRBLleida, Lleida, Spain); Esther Irene Schwarz (Department of Pulmonology and Sleep Disorders Centre, University Hospital Zurich, Zurich, Switzerland); Jonathan E Shaw (Clinical Diabetes and Epidemiology, Baker Heart and Diabetes Institute, Melbourne, Australia); Garima Shukla (Queen's University, Kingston, ON, Canada and Department of Neurology, All India Institute of Medical Sciences, New Delhi, India); Joerg Steier (Centre of Human and Applied Physiological Sciences (CHAPS), Faculty of Life Sciences and Medicine, King's College London, London, UK); John Stradling (NIHR Biomedical Research Centre Oxford, University of Oxford, Oxford, Oxfordshire, UK); Erik Thunström (Department of Molecular and Clinical Medicine/Cardiology, Institute of Medicine, Sahlgrenska Academy, University of Gothenburg, Sweden); Ji-Guang Wang (Department of Hyertension, Ruijin Hospital, Shanghai Jiaotong University School of Medicine, Shanghai, China); Terri E Weaver (College of Nursing; Division of Pulmonary, Critical Care, Sleep & Allergy, Dept. of Medicine, College of Medicine, University of Illinois Chicago,); Antonella Zambon (Biostatistic Unit, IRCCS Istituto Auxologico Italiano, Milan, Italy; Department of Statistics and Quantitative Methods, University of Milano-Bicocca, Milan, Italy); Davide Soranna and Gaia Zambra (Biostatistic Unit, IRCCS Istituto Auxologico Italiano, Milan, Italy).