Spontaneous pneumomediastinum (SPM) was first described by Laennec in 1827,1 and is a rare pathological condition characterized by the presence of free air or gas in the mediastinum. Presumably this is due to alveolar rupture caused by a sudden increase in intra-alveolar pressure, with dissection of tissue along the mediastinal space that can reach the subcutaneous tissue of the neck.2
A 21-year-old male with history of type 1 diabetes mellitus. Symptoms began after omission of a dose of NPH insulin, with subsequent malaise, nausea and repeated vomiting which caused him to seek hospital attention. The patient did not report any history of trauma.
On examination, the patient presented Kussmaul breathing and palpable subcutaneous crepitus in the maxillary region (bilateral), the neck and the anterior thorax to the epigastrium, the posterior thorax to T6, and to the distal third of the arms. Plasma osmolarity was 280mOsm/l with a water deficit of 10l. Blood glucose was 530mg/dl, sodium 135mmol/l, potassium 3mmol/l and chloride 109mmol/l. Arterial blood gas showed a pH of 7.2, pCO2 of 35mmHg, pO2 of 80mmHg, HCO3 of 9meq/l and base excess of −18U. Urinalysis revealed ketonuria (80mg), as well as glucosuria (300mg/l).
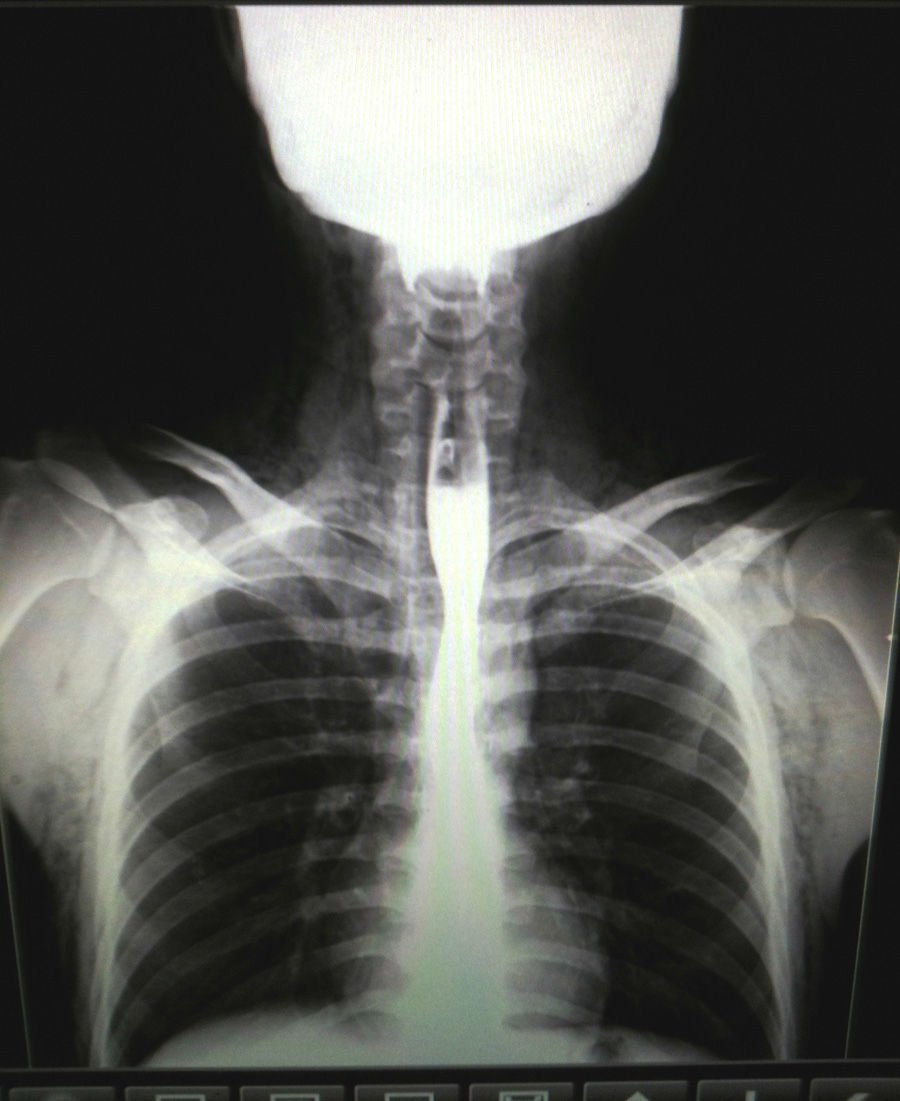
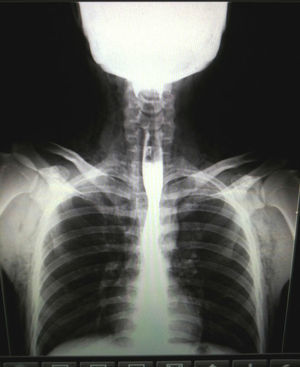
Chest X-ray showed air in the cervical region and in the anterior thorax. Esophagogram ruled out esophageal injury (Fig. 1).
The patient was treated with hydration and insulin, stabilizing after 24h. The extent of subcutaneous emphysema decreased with conservative management; the patient was discharged after 5 days of treatment and on reassessment 15 days later complete resolution of subcutaneous emphysema and SPM was found.
Studies carried out to date are consistent in their results: higher incidence in males (3:1) with a mean age of 20 years. The main symptom is chest pain followed by neck pain, breathlessness and sore throat; the main clinical manifestation is subcutaneous emphysema. Generally, authors agree that chest X-ray is sufficient for diagnosis; however, CT scan, radiological studies of the neck or water-soluble contrast esophagraphy can be used in order to rule out other alterations. Although some authors report recurrence in SPM, it is generally considered non-recurring, and therefore long-term monitoring is unnecessary.1
The pathophysiology is unknown; in ketoacidosis, increased alveolar pressure may be due to emetic exertion or Kussmaul breathing, and this hyperpneic phenomenon is considered to be secondary to metabolic acidosis. The accumulation of air between the anterior parietal surface of the pericardium and the anterior surface of the chest could produce crepitus synchronous with the heartbeat, perceived on auscultation over the cardiac apex and left sternal border. This pulmonary hyperinsuflation, therefore, causes alveolar damage with subsequent leakage of air through the alveolar spaces into the interstitium, which is then transported along the bronchovascular sheaths into the mediastinum, which can result in subcutaneous emphysema.3
While our patient responded favorably to a conservative approach, management with orotracheal intubation and mechanical ventilation may be required.4
We intend to contribute to existing literature on SPM, the incidence of which is so low that it may be under-diagnosed. The condition, however, is self-limiting and patient prognosis is good in most cases.
Please cite this article as: Flores López EN, Álvarez Torrecilla LC, López Alférez R. Neumomediastino espontáneo en un paciente con cetoacidosis diabética: reporte de un caso. Arch Bronconeumol. 2014;50:459.