There is mounting evidence that pulmonologists can safely and reliably sample lesions located near the esophagus and stomach using an echobronchoscope (EUS-B). These lesions include both supra-diaphragmatic (lung, pleura, pericardium, and mediastinal lymph nodes—LN—) and infra-diaphragmatic locations (left adrenal gland—LAG—, liver, pancreas, and retroperitoneal LN).1 Nevertheless, there is no documented evidence of EUS-B-guided fine-needle aspiration (EUS-B-FNA) of a right adrenal gland (RAG).
We present a case of an 82-year-old non-smoker woman who was referred to the pulmonary department for asthenia and hemoptysis.
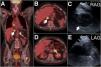
CT and PET scans showed a 48mm×40mm right mediastinal-hilar mass, with a maximum standard uptake volume (SUV) of 25.8 and a few subcentimetric LN at 4R (SUV of 5.1) and 11R (SUV of 4.9). Additionally, they revealed bilateral adrenal lesions (right: 23mm, SUV of 22.7, and left: 28mm, SUV of 19.9), as well as a left femur lesion (SUV of 16.1) (Fig. 1).
An endobronchial ultrasound (EBUS) was initially performed, sampling the 4L LN and the mediastinal mass. In the same sitting, the procedure was completed via the esophagus with the same EBUS scope (EB19-J10U, Pentax). At the level of the lesser curvature of the stomach a 19.7mm heterogeneous lesion in the RAG was visualized. Three punctures were made with a 22-gauge needle (SonoTip EBUS ProFlex, MediGlobe). Similarly, an EUS-B-FNA of the LAG (14.1mm) was performed. The entire procedure was completed in 33min without any complications.
The anatomic pathology findings of the RAG showed numerous medium-to-large atypical cells, which were positive for TTF-1. The molecular study was positive for the p.L858R mutation in EGFR, thereby rendering the patient eligible for treatment with tyrosine-kinase inhibitors. The PD-L1 expression was weakly positive (<50%).
These findings were consistent with metastasis of pulmonary adenocarcinoma. The results of both the LAG and the mediastinal mass biopsies were comparable. 4L was negative for malignancy.
The clinical stage was determined to be IVB, based on the 9th edition of the TNM classification for lung cancer (9th TNM). The tumor committees proposed the initiation of treatment with Osimertinib.
Adrenal metastases are present in 8% of metastatic lung cancers. It is possible to perform EUS-B to complete extra-thoracic staging during a single procedure and this is a feasible and safe (0.2% minor complications, no major complications)2 procedure recommended by international guidelines. Moreover, it may have a significant impact on the treatment plan3 and may obviate the need for multiple supplementary procedures.
Due to its anatomical location (typically in close proximity to the second part of the duodenum), RAG is not usually accessible to EBUS, and thus is not included in lung cancer staging recommendations or guidelines. The puncture of the RAG with an echoendoscope has been previously described,4 however, even by gastroenterologists the access to the RAG is more challenging than that of the LAG.
An alternative approach to the adrenals is CT-guided percutaneous puncture, which has been associated with a higher reported complication rate (2.5%).
Nevertheless, if accessible, it is crucial to confirm the location and number of extrathoracic metastases, particularly considering the proposed changes in the 9th TNM,5 as these may influence prognosis.
In conclusion, this is the first report to confirm a right adrenal metastasis using an echobronchoscope and performed by a pulmonologist.
Authors’ contributionsStudy concept and design, JCH. Acquisition of data, JCH, JLG, IS. Drafting of the manuscript, JCH. Critical revision of the manuscript for important intellectual content, JCH, JLG, IS.
Informed consent formThe patient has signed the informed consent form.
Conflict of interestsThe authors state that they have no conflict of interests.
Dr. Rosa Cordovilla (Interventional Pulmonology Unit) and Dr. Antonio Velasco and Dr. Alberto Álvarez (Endoscopy Unit) of the University Hospital of Salamanca, for all the tips on the EUS-B technique.
Dr. Francisco López, Dr. Lucía García-Alfonso, Dr. Miguel Ariza (IP Unit, HUCA) for all their advice.
Dr. Luis Fernández, Dr. Héctor Torres (Pathology Department, HUCA) for the analysis of the samples.
Inmaculada Sánchez and María Gil (Nurses, IP Unit, HUCA) for taking care of the patient.