The authors describe a case of an 82-year-old male, heavy smoker, with a 1-month history of several syncopal episodes that performed a transthoracic echocardiogram as an outpatient that showed a left atrial mass suggesting a myxoma. The patient was admitted for etiologic study. A full blood count showed normocytic and normochromic anemia.
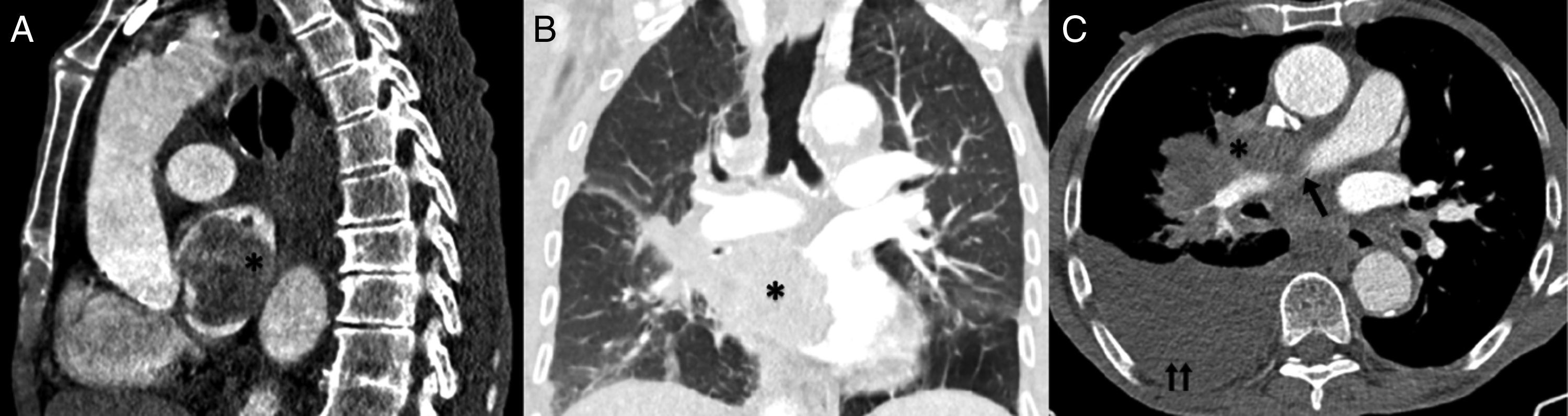
A thoracic computer tomography showed a right hilar, heterogenic and vascular mass with 101mm×45mm invading the left atrium (Fig. 1). The mass obliterates the right pulmonary vein and involves the right pulmonary artery with obliteration of the segmental branches of the middle lobe and compression of the segmental branches of the right inferior lobe. The posterior side of the right atrium and the distal portion of the superior vena cava showed also signs of invasion. Multiple bilateral pulmonary nodules suggesting secondary lesions and multiple mediastinal adenopathies were found. There were no bone lesions suggesting bone metastasis.
Sagittal (A) and coronal (B) CT scan showing the pulmonary mass invading the left atrium. Axial CT (C) showing the right pulmonary artery involved by the mass and an unilateral large-volume pleural effusion.
*: pulmonary mass; arrow: right pulmonary artery; double arrow: right pleural effusion.
Although no malignant cells were found in the pleural fluid and pleural biopsy analysis, a stage IV lung cancer diagnosis was assumed by a multi-disciplinary lung cancer group. Due to the severity of the lesions and the high risk of procedure-related complications, the multi-disciplinary group considered that there was no benefit of invasive diagnostic or therapeutic procedures and a best care support was decided for this patient.1