Solid organ transplant recipients have an increased risk of developing malignancies, particularly lung transplant recipients, being one of the leading causes of morbidity and mortality.1,2 Certain viral infections are related with the development of tumours, both in immunocompetent and immunosuppressed patients.1,4 In the latter, the permanent state of immunosuppression, makes them more susceptible to new infections or reactivations1,3 such as by human herpesvirus 8 (HHV-8), which is associated with Kaposi Sarcoma (KS) and can manifest in very different ways,3,4 as it will be described.
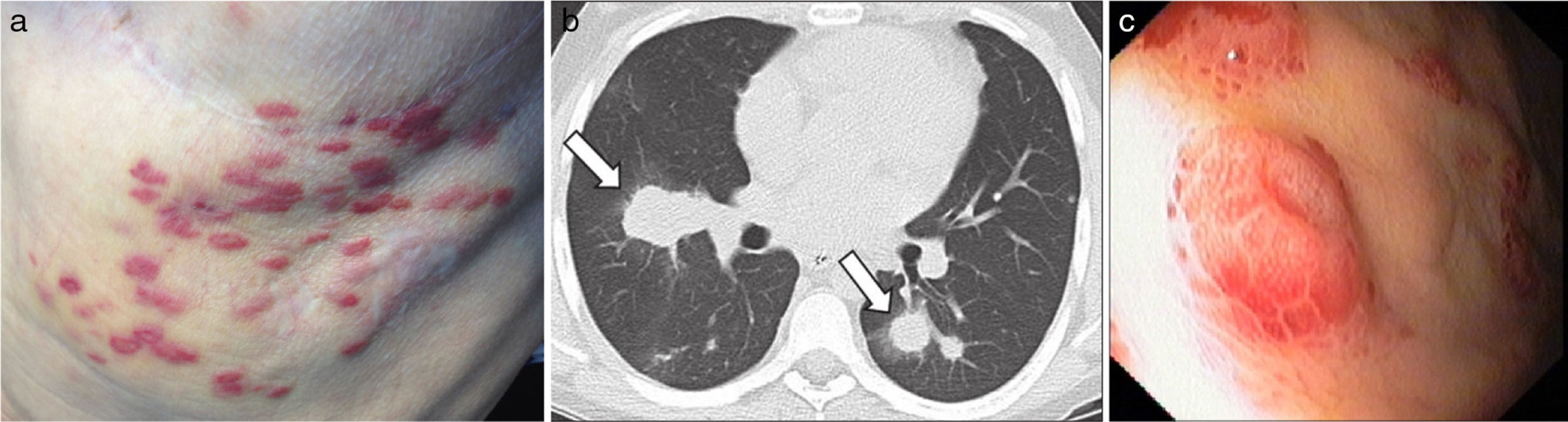
The first case refers to a 63 years old male patient, former smoker, submitted to bilateral pulmonary transplant (BPT) when he was 61 years old. Eleven months after transplant, on a routine visit, two small purpuric skin lesions in the patient's chest were identified. He was referred to the Dermatology outpatient department and clinical vigilance was decided. Five months later, due to progression of the skin lesions, (Fig. 1a), he was submitted to cutaneous biopsy whose pathology revealed morphological features and HHV-8 positive cells, compatible with KS, and its digestive tract involvement was excluded. Meanwhile, he showed functional decline and the diagnosis of bronchiolitis obliterans was made, leading to changes in his immunosuppression from mycophenolate mofetil 1250mg bid to everolimus 0.5mg bid. Afterwards, he presented clinical worsening with dyspnoea, bilateral pulmonary infiltrates and respiratory failure without response to non-invasive ventilation, all portrayed as a possible pulmonary involvement by KS, associated with transplant rejection (Fig. 1b). The patient died two days after these symptoms began, without having started specific therapy for KS.
The second case describes a 35 years old male patient with bronchiectasis of unknown aetiology, submitted to BPT at the age of 30. Regarding post-transplant complications, the authors emphasise acute rejection with progression to bronchiolitis obliterans with functional stability without respiratory failure. He begun immunosuppression with everolimus 0.5mg bid and tacrolimus 4.5mg bid. Fifty months after transplant, he was hospitalized for both prostatitis and acute cholecystitis. During that period the patient presented severe anaemia (haemoglobin 6.8g/dL) and he underwent endoscopic study which revealed multiple, vascular, round and elevated lesions dispersed in the stomach, suggestive of KS (Fig. 1c). The histological examination confirmed this suspicion after the identification of positive cells to HHV-8 and its serology was negative. Few days later, the patient died after the onset intra-abdominal sepsis.
KS in lung transplant patients has been rarely described in literature, contrary to other solid organ recipients.2,4 Different clinical expressions and severity can occur, but usually they are aggressive, commonly involve skin and visceral organs3,4 and time from transplantation to diagnosis can vary widely (3•124 months).3 KS related to immunosuppression usually disappears with mTOR inhibitors5 or with modification, reduction or cessation of immunosuppressive drugs, which in lung transplant patients is not recommendable due to loss of the graft,3 making their therapeutic approach a challenge. Unfortunately, clinical deterioration in both patients did not allow us to start specific therapy for KS.
FundingNone to declare.
Conflict of InterestsThe authors declare that there is no conflict of interests directly or indirectly related to the contents of the manuscript.
The authors are grateful to the staff of the pulmonology department and all physicians at Centro Hospitalar São João involved in these two cases.