Obstructive sleep apnea-hypopnea syndrome (OSAHS) is very prevalent in children and adolescents,1 and short- and long-term complications are significant, the most important being neurocognitive impairment,2 learning difficulties,3 and cardiovascular and metabolic changes. Myelination and neural connectivity during neural development in infancy may be affected by OSAHS, and this is why an accurate diagnosis of OSAHS is especially important in this age group.
For decades, however, the diagnosis of OSAHS in children and adolescents has been problematic. Clinical manifestations and physical examination are poor predictors of OSAHS.4 Habitual snoring, a cardinal symptom of OSAHS, is a warning sign, but this symptom alone is insufficient to predict whether the patient is at risk of developing OSAHS. The difficulty in obtaining an accurate diagnosis from clinical signs and symptoms is further compounded by diagnostic recommendations that currently designate nocturnal polysomnography (PSG) as the gold standard for the diagnosis of OSAHS in children. While PSG has historically been the technique of choice in the diagnosis of OSAHS, it presents a series of limitations, such as restricted availability (not all centers that see children with OSAHS have access to this test), high cost, more intensive use of resources, and the need for specialized technicians and physicians to administer the test and interpret the results, respectively. Waiting lists for PSG vary all over the world, but children with OSAHS generally wait too long for a diagnosis.
In view of these problems, a number of studies have been performed in the last 20 years to investigate the validity of different diagnostic tests. These include tonsil size,5 video or audio recordings, questionnaires,6,7 lateral neck X-ray, pulse oximetry, cardiorespiratory polygraphy8 and, in recent years, plasma and urinary markers.9 Most of these tests were analyzed in a systematic review published by our group a few years ago.4 In this review, we identified 965 potentially relevant studies that sought to compare other types of test with the gold standard, i.e., PSG, in the diagnosis of OSAHS in children. Of the 33 studies finally selected,4 only 13 used the currently accepted consensus definition of OSAHS, namely, an apnea/hypopnea index (AHI) >1.0/h.4 This definition, however, should be used with caution in older age groups (adolescents) and in groups with special OSAHS phenotypes. As well as AHI, other factors, such as oxygen saturation, may be useful in the diagnosis of OSAHS.
The remarkably large number of studies initially identified in this systematic review is symptomatic of the widespread concern in the scientific community regarding this topic. However, very few studies followed the recommended methodology, insofar as most either failed to compare their diagnostic test with the reference PSG, or used other definitions of OSAHS, and this affected the accuracy of the diagnosis.4 Of the tests that achieved high diagnostic accuracy, the most interesting were cardiorespiratory polygraphy10 and urinary biomarkers.11 Questionnaires and other simplified tests, such as home video recording, only achieved moderate diagnostic accuracy. The diagnostic yields of lateral neck X-ray and general physical examination were unacceptable, and these techniques were subsequently excluded from the meta-analysis.4
Cardiorespiratory polygraphy proved to be a promising test in the diagnosis of OSAHS in children.4,10 In a systematic review published by our co-author, this test achieved a global diagnostic concordance of 84.9%, which increased to 95% in a subgroup of children aged 6–14 years.10 This has validated cardiorespiratory polygraphy performed in the sleep laboratory as a less invasive, more convenient and more cost-effective technique than PSG. Some years later, this study was followed up with a home-based trial, which achieved a sensitivity of 90.9% and a specificity of 94.1%.8 Other more recent studies have confirmed these results using a large variety of methods, underlining the need for simplified studies.12 Studies performed by our group have shown that signal loss and artifacts in the cardiorespiratory polygraphy are infrequent, and 93%–94% were correctly interpreted at the first attempt.13 Despite the reliability of this technique, some limitations must be taken into account, particularly with regard to the high percentage of false negatives in milder cases. Despite this limitation, there is little doubt that cardiorespiratory polygraphy is a good alternative if PSG is unavailable,14 and this technique has been accepted by Spanish guidelines for some years now.15 Nevertheless, some care must be taken: when results are negative and symptoms persist, the study should be repeated or a PSG should be performed, if possible. The American Sleep Academy recently published a consensus that advises against home cardiorespiratory polygraphy in children; unfortunately, they do not suggest any alternative solutions.16
Urinary biomarkers achieved the highest diagnostic accuracy in the above-mentioned systematic review.11 Using specific laboratory techniques, certain molecules could be identified in children with OSAHS (uromodulin, urocortin 3, orosomucoid 1, and kallikrein) that were not present in the controls. The diagnostic accuracy of these biomarkers was almost identical to that of PSG (sensitivity and specificity close to 100%).11 We believe these non-invasive, easily accessible screening techniques are promising and, once they are widely available, will probably constitute one of the most cost-effective solutions for the diagnosis of OSAHS in the long term. Biomarkers appear to be particularly useful in identifying children with OSAHS who are at risk of developing neurocognitive consequences.17 The ability to predict the consequences of OSAHS is one of the most important benefits of these type of tests, particularly considering the limitations of PSG in this respect.
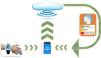
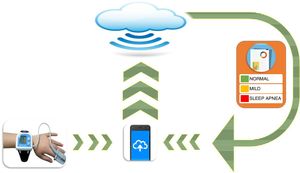
In addition to polygraphy and biomarkers, interest in simple, single-point tests such as pulse oximetry has recently been revived after having fallen into disrepute for years. A recent critical review of the literature18 evaluated criteria and considerations associated with the use of pulse oximetry, and arrived at the conclusion that this method is valuable in situations in which PSG or other methods are not readily accessible. Even so, the main problem with all these diagnostic techniques lies in their limited scalability. Two different groups have attempted to overcome this problem and improve usability, particularly in less expert settings, with very promising results. A recent multicenter study in 4190 children found that analyzing nocturnal pulse oximetry parameters using an automated neural network algorithm derived through machine learning and artificial intelligence approaches had excellent diagnostic sensitivity and specificity.19 The scalability of this new analysis technique (Fig. 1) has helped pulse oximetry reemerge as a diagnostic tool that may be useful in screening, particularly in centers with limited access to sleep studies such as polygraphy or PSG.
In summary, we are impressed by the progress made in OSAHS diagnostics in children. The use of tests such as polygraphy, pulse oximetry, and biomarkers, is supported by increasingly solid, promising evidence. These new techniques can and should be used to speed up the diagnostic process, since it is clear that children with OSAHS must not linger on waiting lists resulting in a late diagnosis. The future has arrived, and it is time to move forward.
FundingDG receives financial support in his position as the Herbert T. Abelson Professor of Pediatrics and research funding from the National Institutes of Health grant no. HL130984.
Please cite this article as: Brockmann PE, Alonso-Álvarez ML, Gozal D. Diagnóstico del síndrome de apnea hipopnea del sueño en niños: pasado, presente y futuro. Arch Bronconeumol. 2018;54:303–305.