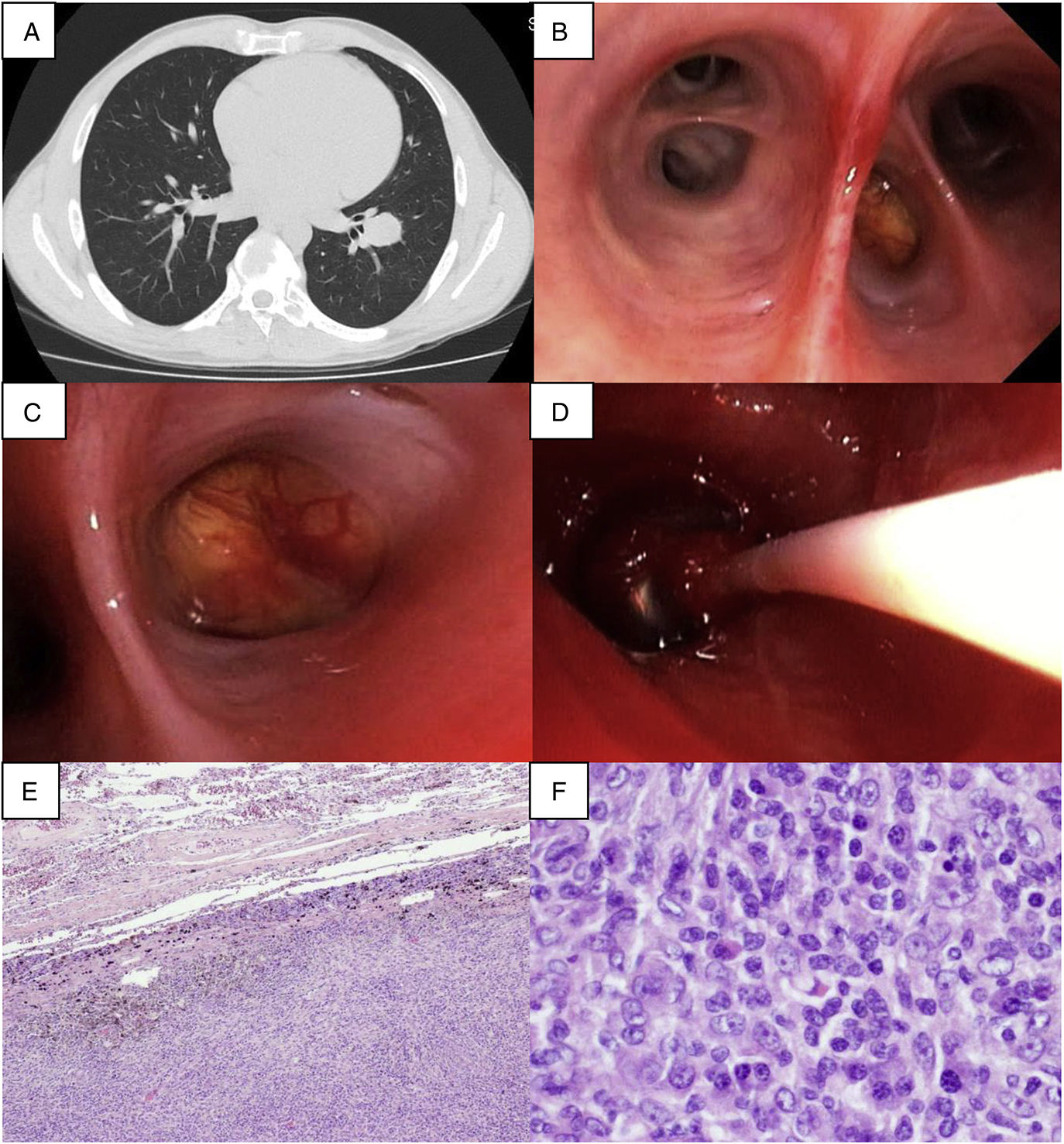
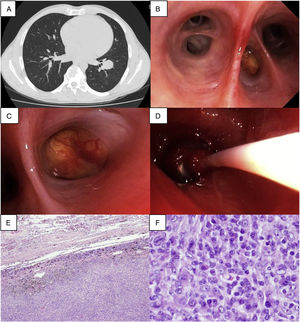
A 41-year-old man, former smoker, presented with a 3-month history of a non-productive cough. Although Lab disclosed mild thrombocytopenia there was no history of hemoptysis. Chest CT revealed a 29mm homogeneous nodule in the left lower lobe (LLL, Fig. 1A). Bronchoscopy showed the presence of a yellowish hypervascularized mass at LB9 (Fig. 1B and C). The first biopsy immediately unleashed a profuse bleeding, which despite maintaining the wedging position and lavage with cold saline and aminocaproic acid instillation could not be controlled. A balloon catheter tamponade was inserted at the common basal trunk (Fig. 1D). However, severe bleeding persisted whenever the balloon was deflated. Patient was then intubated with reinsertion of the balloon tamponade, enabling clinical stabilization until emergency left lower lobectomy was performed, with uneventful recovery. Pathologic surgical report revealed an inflammatory myofibroblastic tumour (IMT, Fig. 1E and F). Presently the patient has no clinical complaints.
(A) Chest CT (axial plan (AP)): a 29mm homogeneous nodular lesion in the left lower lobe; (B) Endobronchial view of left lower lobe, with a mass blocking the lateral segmental bronchus (LB9); (C) A closer view of the mass, which was yellow, with a smooth surface and a long implantation base, containing multiple superficial vessels, almost completely blocking the entrance orifice of LB9; (D) The balloon catheter tamponade was inserted at the left common basal trunk; (E) Microscopic examination of the surgical sample revealed tumour free margins and (F) formation of aggregates with plenty of plasma cells and cells having an oval to fusiform appearance.
IMT is an extremely rare low-grade tumour, with true benign or past inflammatory aetiology, more common in children and young adults. Complete resection is the main treatment choice, providing a good survival.1,2
Lobectomy was carried out because massive bleeding prevented a less aggressive approach. This case highlights the need to anticipate the difficulties and to decide procedure sequence to handle them.