The management of bronchiectasis, particularly exacerbations, places a significant burden on healthcare systems, causing frequent hospital admissions and lengthy hospital stays.1
Chronic bronchial infection (CBI) by Pseudomonas aeruginosa (PA) affects 9–31% of patients with bronchiectasis and is associated with worse prognosis and quality of life, and an increased frequency of exacerbations.2,3 Antibiotic therapy is efficacious in reducing the number of exacerbations, time to first exacerbation, sputum purulence, and breathlessness, and is recommended by national and international guidelines.4,5
Colistin is an antibiotic of the polymyxin group with inhibitory potential against Gram-negative bacteria, including PA. Several studies showed the efficacy of colistin in patients with different respiratory disorders, but a limited number has been conducted in non-cystic fibrosis (NCF)-bronchiectasis.6
This study assessed treatment adherence to nebulised colistin administered with the I-neb device and the impact of colistin treatment in clinical outcomes in patients with NCF-bronchiectasis and CBI by PA.
This multicenter, observational, prospective cohort study was conducted at 11 Spanish centres. The study adhered to the tenets of the Declaration of Helsinki and was approved by the Ethics Committee of Jaén. All participants provided written informed consent. Clinical data were collected prospectively for up to 12 months, with the exception of treatment adherence, which was only retrieved after 6 months as prespecified in the protocol.
Participants were aged ≥18 years, with bronchiectasis diagnosis confirmed by high-resolution computed tomography of the chest and CBI by PA,7 and who started treatment with nebulised colistin for ≥6 months. Patients were excluded if presented a previous diagnosis of CF.
Participants received colistin (Promixin®; Zambon Company S.p.A., Italy) at 1 million international units administered twice a day via the I-neb Adaptive Aerosol Delivery (AAD) system (Philips Respironics, Chichester, UK) according to routine clinical practice.
The primary objective was to assess treatment adherence to nebulised colistin administered with the I-neb device. Overall adherence is the proportion of doses initiated among the total prescribed. Compliance is the proportion of nebulisations initiated that were completed (dose delivery duration ≥2min). True adherence shows the proportion of doses properly administered ([% adherence×% compliance]/100).
Microbiological response, lung function, number of exacerbations and hospital admissions and the change in bronchiectasis severity after 12 months of colistin treatment were evaluated as secondary endpoints.
Spirometry was conducted to determine the forced expiratory volume in 1 second (FEV1) and forced vital capacity (FVC) according to standard guidelines.8 The degree of dyspnoea was measured with the Medical Research Council (MRC) dyspnoea scale.9 The number of lobes involved was assessed with high-resolution computed tomography. Exacerbations were defined based on the Spanish Society of Pulmonology (SEPAR) guideline.7
To determine the severity of bronchiectasis, we used the FACED (FEV1, Age, Colonisation, Extension, Dyspnoea, 0–7 scale),10 E-FACED (E, Exacerbations, 0–9 scale)11 and Bronchiectasis Severity Index (BSI, 0–26 scale)12 scoring systems.
For the sample size calculation, we considered a prevalence for NCF-bronchiectasis of 200 cases per 100,000 inhabitants,13–15 of which 10–30% would have a chronic bronchial infection by PA. Based on a population of 3.75 million people aged>18 years among participating centres,16 a sample size of 130 participants would have a 9% precision to estimate the proportions using a normal asymptotic confidence interval with a Finite Population Correction Factor for a two-sided 95% CI and assuming 10% drop-out rate.
Statistical analyses were conducted using the Statistical Package for Social Sciences (SPSS) software for Windows, version 22.0 (Chicago, IL, US) with a two-tailed level of significance α=0.05.
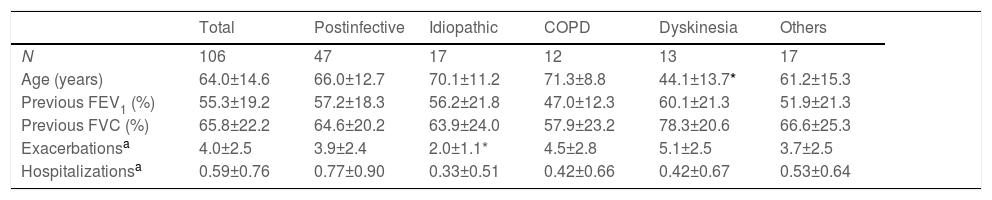
A total of 126 patients were included in the study and data from 106 were analysed. Demographic and clinical data are presented in Table 1. Patients with ciliary dyskinesia were significantly younger than the overall population (p<0.001), and those with idiopathic bronchiectasis had significantly fewer exacerbations (p<0.021) (Table 1).
Baseline demographic and clinic characteristics in patients with non-cystic fibrosis bronchiectasis classified by aetiology group.
| Total | Postinfective | Idiopathic | COPD | Dyskinesia | Others | |
|---|---|---|---|---|---|---|
| N | 106 | 47 | 17 | 12 | 13 | 17 |
| Age (years) | 64.0±14.6 | 66.0±12.7 | 70.1±11.2 | 71.3±8.8 | 44.1±13.7* | 61.2±15.3 |
| Previous FEV1 (%) | 55.3±19.2 | 57.2±18.3 | 56.2±21.8 | 47.0±12.3 | 60.1±21.3 | 51.9±21.3 |
| Previous FVC (%) | 65.8±22.2 | 64.6±20.2 | 63.9±24.0 | 57.9±23.2 | 78.3±20.6 | 66.6±25.3 |
| Exacerbationsa | 4.0±2.5 | 3.9±2.4 | 2.0±1.1* | 4.5±2.8 | 5.1±2.5 | 3.7±2.5 |
| Hospitalizationsa | 0.59±0.76 | 0.77±0.90 | 0.33±0.51 | 0.42±0.66 | 0.42±0.67 | 0.53±0.64 |
Data are expressed as mean±SD or (%).
The overall adherence rate was 86.8%, true adherence 84.3% and compliance 96.6%. Most patients achieved overall and true adherence rates above 80% (75.5% and 73.6%, respectively), and 97.2% of patients completed>80% of nebulisations.
The proportion of patients with PA isolates decreased over time, showing a 62.3% reduction after 12 months. The rate of patients with detected levels of other pathogens generally decreased from baseline over the follow-up.
FEV1 increased by 4.4% (p<0.001), the total number of exacerbations showed a 63.4% reduction (p<0.001) and hospital admissions a 54.9% reduction (p<0.001) after 12 months of colistin treatment (Table 2).
Change in exacerbations, hospital admissions and lung function after 6 months of treatment with nebulised colistin in patients with non-cystic fibrosis bronchiectasis.
| Baseline(N=106) | Month 12(N=86) | p-Value | |
|---|---|---|---|
| FEV1 (%) | 55.3±19.2 | 59.7±22 | <0.001 |
| Total exacerbations (per patient), n (mean±SD) | 344 (4.0±2.5) | 126 (1.5±1.3) | <0.001 |
| Total hospital admissions (per patient), n (mean±SD) | 51 (0.6±0.8) | 23 (0.3±0.6) | <0.001 |
Data are expressed as mean±SD, % or n (number).
FEV1, forced expiratory volume in 1s.
After 12 months of colistin treatment, the FACED and E-FACED prediction scores showed a decreased proportion of patients classified as moderate-severe (17.2% reduction with FACED and 21.7% with E-FACED) and the BSI showed a 54.2% reduction in patients classified as severe.
In this prospective study, patients treated with nebulised colistin showed excellent adherence rates, improvement in microbiological control, lung function and disease severity, and a reduction in the number of exacerbations. The study population comprised patients with NCF-bronchiectasis, who mostly presented moderately severe lung impairment17 and frequent exacerbations.
We observed high adherence (84.3%) and compliance rates (96.6%) to nebulised colistin administered with the I-neb device. These rates were higher than some reported in patients with NCF-bronchiectasis, although only a limited number of studies have addressed treatment adherence to antibiotic therapy in this population. In a randomised controlled trial, >90% adherence to nebulised colistin administered through the I-neb device was achieved by 61.4% of patients.6 Similarly, a significant decrease in the number of patients with PA isolates was detected, which was higher than eradication rates observed in previous observational studies with colistin.18,19 Exacerbations were reduced by 63.4% and hospital admissions by 54.9% after 12 months of treatment. These results support those observed in a randomised controlled trial6 and an observational study.19 Of remarkable importance is the improvement in lung function after 12 months of treatment (FEV1: 55.3% at baseline and 59.7% after 12 months). Since bronchiectasis is an irreversible and chronic process, we would expect clinical improvement without significant functional changes. Indeed, previous studies with nebulised antibiotics failed to demonstrate an improvement in lung function.6,20
This study is one of the few reporting the effectiveness of nebulised colistin administered with the I-neb device and, to our knowledge, the only one assessing treatment adherence, pathogen clearance and disease severity in this population. The main strengths of this study are the considerable sample size analysed (106 patients) and long-term follow-up (up to 12 months). Compared with studies evaluating the effect of nebulised colistin in NCF-bronchiectasis, only the study of Haworth et al. was carried out on a larger population (149 patients), but during a shorter follow-up.6
This study presents several limitations. First, its observational design and the lack of comparator limit proving direct causality. Second, treatment adherence was not assessed after 12 months of colistin treatment. Third, we did not consider the impact of treatment burden on adherence at baseline.
Author's contributionsBNB, FCM, APG, EGMM, MAG, JCBR, RJG, MSCG, JLLC, SMN, AVM, JMVB contributed substantially to the study design, data analysis and interpretation, revised the manuscript and approved its final version. BNB, FCM, and JMVB supervised the study. FCM supervised the statistical analysis of the study.
FundingThis study was supported by Neumosur and Zambón. Laboratorios Praxis provided statistical and data analysis support.
Conflict of interestFCM, APG, and JMVB participated in advisory boards, symposia, and received funding to conduct studies outside the present work from Zambón, Chiesi and Laboratorios Praxis.
The authors thank Laboratorios Praxis for statistical and data analysis assistance. Laboratorios Praxis did not contribute to the study design, data analysis or manuscript preparation. Carla Granados of Trialance SCCL provided medical writing assistance.