Tracheobronchial injury (TBI), is a rare but life-threatening clinical condition. It can be produced by blunt or open trauma of the cervical and thoracic regions, or by iatrogenic causes, including tracheal intubation, tracheotomy, bronchoscopy, tracheal and bronchial stent placement.1 In this article, we present a case of iatrogenic TBI that was repaired using a synthetic dural graft.
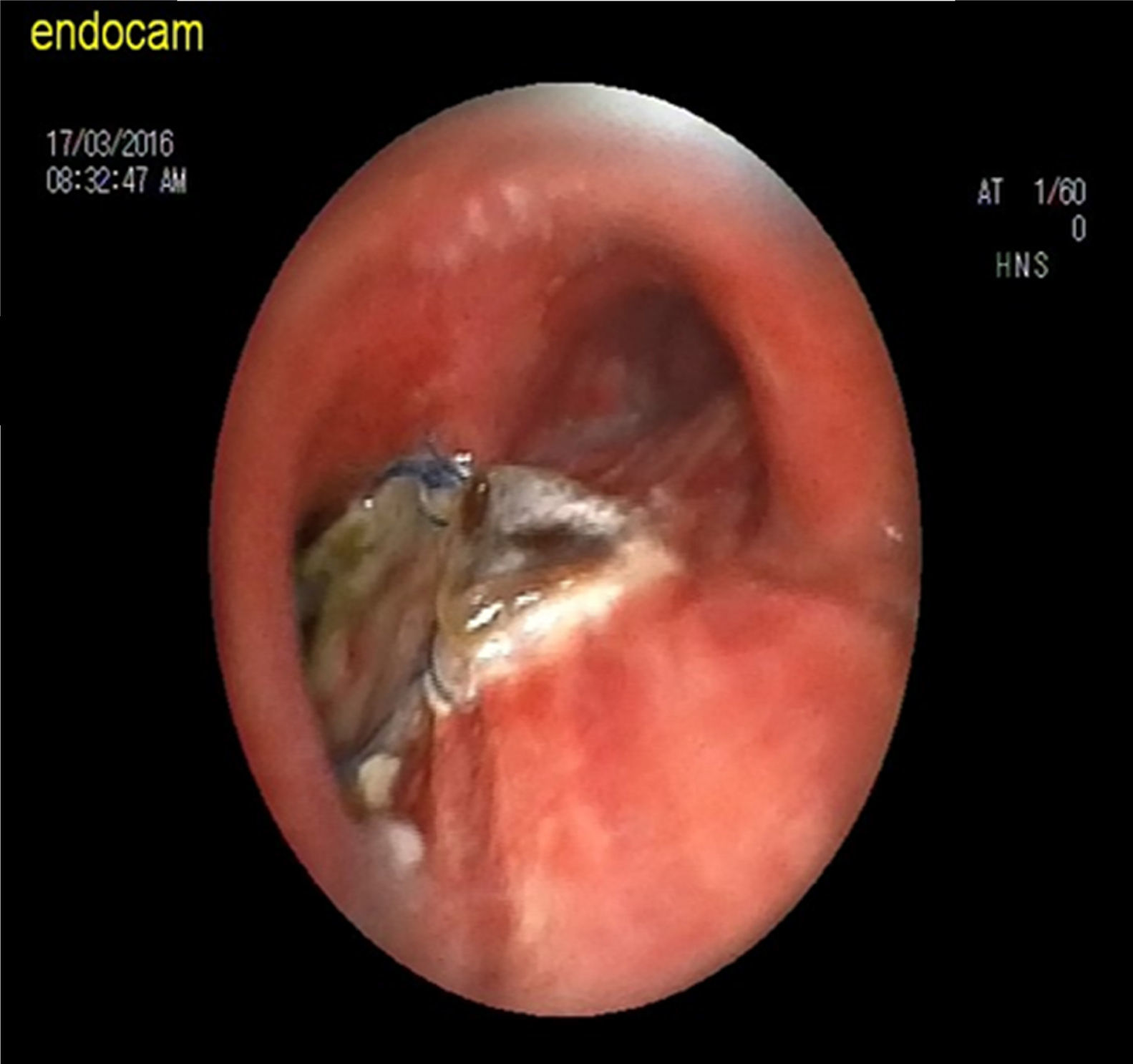
A 62-year old man presented in our hospital with weight loss and difficulty in swallowing. He was admitted to the general surgery unit and underwent gastroscopy, which revealed an ulcerated, fragile, bleeding lesion in the upper third of the esophagus. Histological study of the biopsy sample showed an epidermoid carcinoma. The patient agreed to undergo surgery. Preoperative left posterolateral thoracotomy performed to mobilize the esophagus led to a massive air leak, hypoventilation and desaturation. Emergency evaluation of the patient in the operating theater by the thoracic surgery consultant revealed a rupture. Primary repair of the injury was impossible due to a severe stricture observed in the left upper bronchus caused by cartilage tissue loss in the trachea. Given the state of emergency, a synthetic dural graft (polyethylene terephthalate, dimethyl siloxane) was placed on the injured area and anastomosed with 4/0 polyproylene suture. The graft line was reinforced with fibrin sealant and the application of a composite mesh. After oxygenation, an end-to-end anastomotic stapler was used to reconnect the proximal esophagus to the stomach fundus. The patient was discharged from the hospital 15 days after surgery, and was followed up at 2 and 3 months with fiber optic bronchoscopy (FOB) to evaluate the tracheobronchial lumen and graft (Fig. 1). The graft remained intact with no air leakage and no narrowing at the distal third of the trachea, carina and proximal left main bronchus. The patient is still being followed-up at our clinic.
Eighty percent of TBI's occur around the carina, mainly in the left main bronchus.2 Primary surgical repair is the treatment of choice. However, based on clinical and endoscopic findings, conservative treatment can be employed in some cases.3 In our case, a rupture measuring approximately 3cm was observed in the left distal trachea, carina and cartilage and membranous portions of the left main bronchus, with a width of 1cm in the carina, necessitating the use of the synthetic dural graft.
Bostanci et al. reported repairing a 7cm rupture of the membranous trachea with a pleural patch and vascular graft.4 In our case, a review of the literature did not yield any reports of TBI repair with synthetic dural graft.
We present this case to show that a synthetic dural graft, which is durable, water tight and highly elastic, can be a good alternative for TBI repair under appropriate conditions.