Primitive neuroectodermal tumors (PNETs) and Ewing sarcoma are small round-cell tumors of soft tissues and bones with immunohistochemical and molecular similarities, reason why they have been categorized in the group of Ewing family tumors. PNETs can arise from primitive nerve cells of the central nervous system or outside the central nervous system, called peripheral PNETs.1 Peripheral PNETs within the thoracopulmonary region were originally reported by Askin et al. in 1979,2 and since then they have been defined as Askin's tumors.
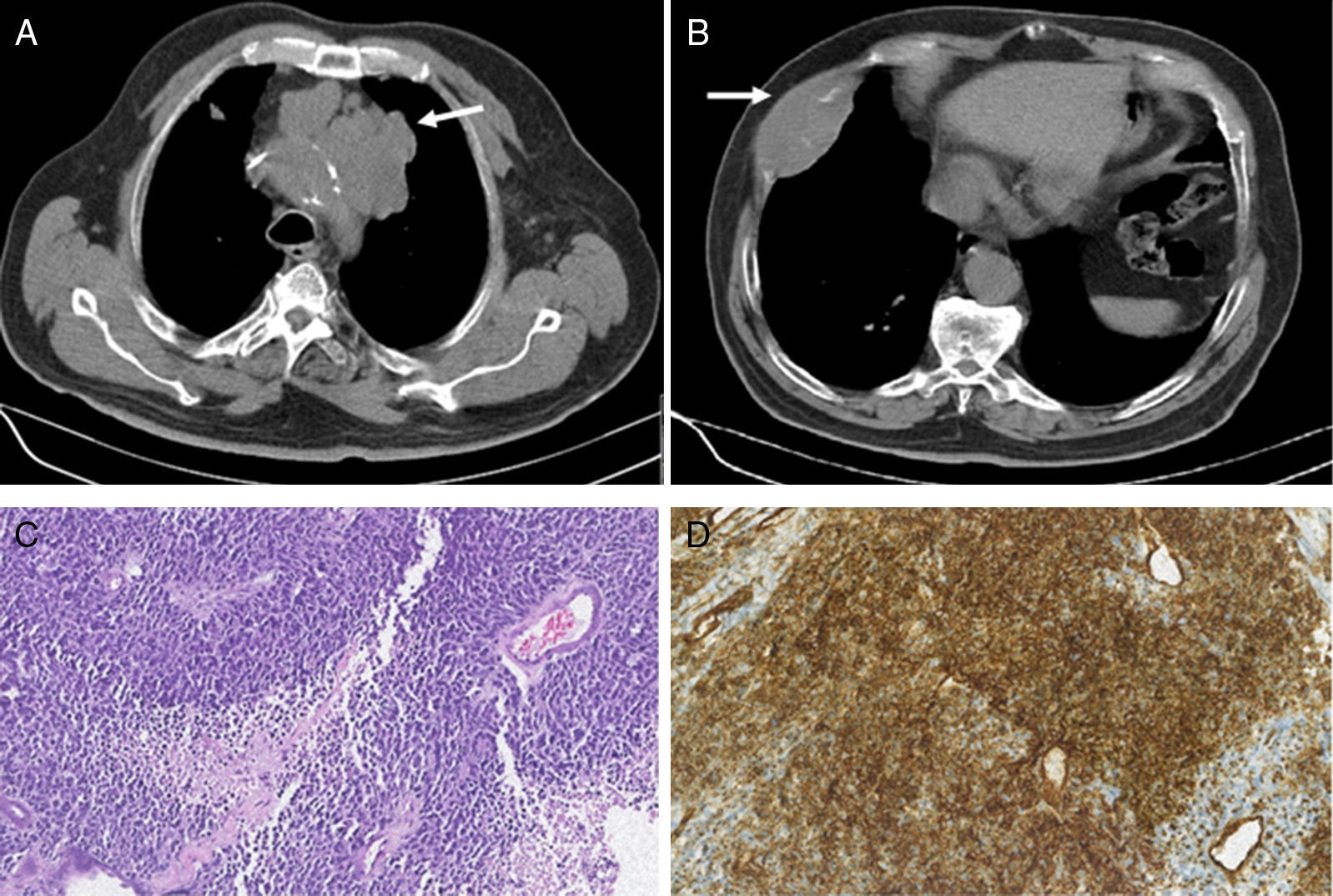
We report the case of a 76-year-old Caucasian man, smoker, admitted to the emergency department with a clinical history of progressively worsening dyspnea, cough and bilateral pleuritic chest pain, asthenia and anorexia, with 6-months evolution. On physical examination, observations were normal, except increased respiratory rate. On inspection and palpation, a hard and painful mass on the right anterolateral hemithorax was detected. Laboratory investigations were normal except for a high lactate dehydrogenase (LDH 944U/L). Chest X-ray revealed bilateral pulmonary opacities and left enlargement of the superior mediastinum. Chest computed tomography (CT) showed three pulmonary masses, one with 6.1cm in the right inferior lobe and two in the left superior lobe (with 5.8 and 2.9cm). The patient also had a pre-vascular solid mass with 9cm in the superior mediastinum (Fig. 1A) and a 7.9cm diameter lytic mass involving the anterior portion of the 7th right rib (Fig. 1B). Eco-guided transthoracic core needle biopsies of the rib lesion were performed and the histopathological examination revealed a small-round cell tumor (Fig. 1C). The immunohistochemistry study was positive to CD99 (Fig. 1D), synaptophysin and vimentine, favoring the diagnosis of Askin's tumor.
(A) Chest CT showing a pre-vascular solid mass with 9cm in the superior mediastinum (white arrow). (B) Chest CT showing a lesion in the anterior portion of the 7th right rib with 7.9cm and bone destruction (white arrow). (C) Photomicrograph illustrating small-sized round cells with scanty cytoplasm. Stain: hematoxylin and eosin (HE); magnification: 20× (D) Immunohistochemistry photomicrograph showing tumor cells positive for CD99; magnification: 20×.
The patient had a hospital-acquired respiratory infection with associated respiratory failure and died, without starting any antineoplastic therapy.
Askin's tumors are rare tumors that develops in the soft tissue of the thoracic wall and mainly occurs in children, adolescents and young Caucasian adults. Reported cases in patients over 60 years are extremely rare.1
Our patient presented some clinical signs and symptoms commonly seen in Askin's tumors, as dyspnea, cough, chest pain, chest wall mass and anorexia. Fever and superficial lymph nodes are other clinical findings reported.2–4 Typical radiographic findings include a large chest mass that can be associated with pleural effusion. Rib destruction is frequent. Pulmonary parenchymal involvement, hilar and mediastinal adenopathies are other associated findings.2,5
If Askin's tumor is suspected, diagnostic confirmation is obtained by histological and immunohistochemical analysis, as was performed in our case. Histological features include small round malignant cells that contain scant cytoplasm. Like the other Ewing's family tumors, Askin's tumor may express neural markers as CD99, neuron-specific enolase, vimentin and Leu7 (CD57). Tumor cells may also be positive for synaptophysin. Diagnostic confirmation can be alternatively made by detection of the typical cytogenetic mutation, a reciprocal translocation between chromosomes 11 and 22 (t[11;22][q24;q12]).5
The ideal treatment of Askin's tumor should be multimodal, and included a combination of neoadjuvant chemotherapy, radical surgical resection and adjuvant chemotherapy and radiotherapy,3,4 however, metastases are frequently seen at the time of diagnosis, making impossible the optimal treatment. Local recurrences after treatment are also frequently seen, reason why Askin's tumor is generally associated with poor prognosis and short survival.
Adverse prognostic factors reported include metastatic disease at diagnosis, larger tumor volume, presence of pleural effusion and poor response to neoadjuvant chemotherapy.4,6 Some studies showed older age to be associated with poorer outcome but other studies showed no association between age and survival.6 Our patient presented several adverse prognostic factors, as metastatic disease and large tumor volume, and we believe that his advanced age had an important contribution to the rapidly fatal evolution after the diagnosis. Early clinical suspicion is crucial, and Askin's tumor must be kept in mind in the differential diagnosis of small round cell malignant tumors of the thorax, even in elderly.