Pneumothorax is a common pleural disease. It is defined as the presence of air in the pleural cavity and results in parenchymal collapse.1 The management of pneumothorax includes observation, simple aspiration, intercostal drainage, intercostal drainage with pleurodesis, or surgical intervention with or without chemical pleurodesis. The form of management is selected depending on the size of pneumothorax, the severity of symptoms, whether there is a persistent air leakage, and comorbidities.2
Pleurodesis is performed in order to achieve symphysis between the 2 pleural layers. Clinically, a variety of sclerosants have been used, including tetracyclin and its derivatives (doxycycline or minocycline), talc, bleomycin, and OK-432.2,3 Currently, talc and OK-432 are most commonly used for pleurodesis in Western countries and Japan, respectively.2 Recently, some studies have reported on the effectiveness of 50% glucose as a sclerosant.4–7 Pleurodesis using a 50% glucose solution is described in the European Respiratory Society task force statement.8 Regarding the side effects of the pleurodesis using a 50% glucose solution, previous reports have described a transient elevation in blood sugar and rapid induction of pleural effusion,4–7 and Takanashi et al. have reported a case of ischemic colitis.9
We used pleurodesis using 50% glucose solution in 11 patients with spontaneous pneumothorax. We encountered 2 cases of treatment-related death due to pleurodesis using a 50% glucose solution, which included acute respiratory distress syndrome (ARDS) and anaphylactic-like reaction.
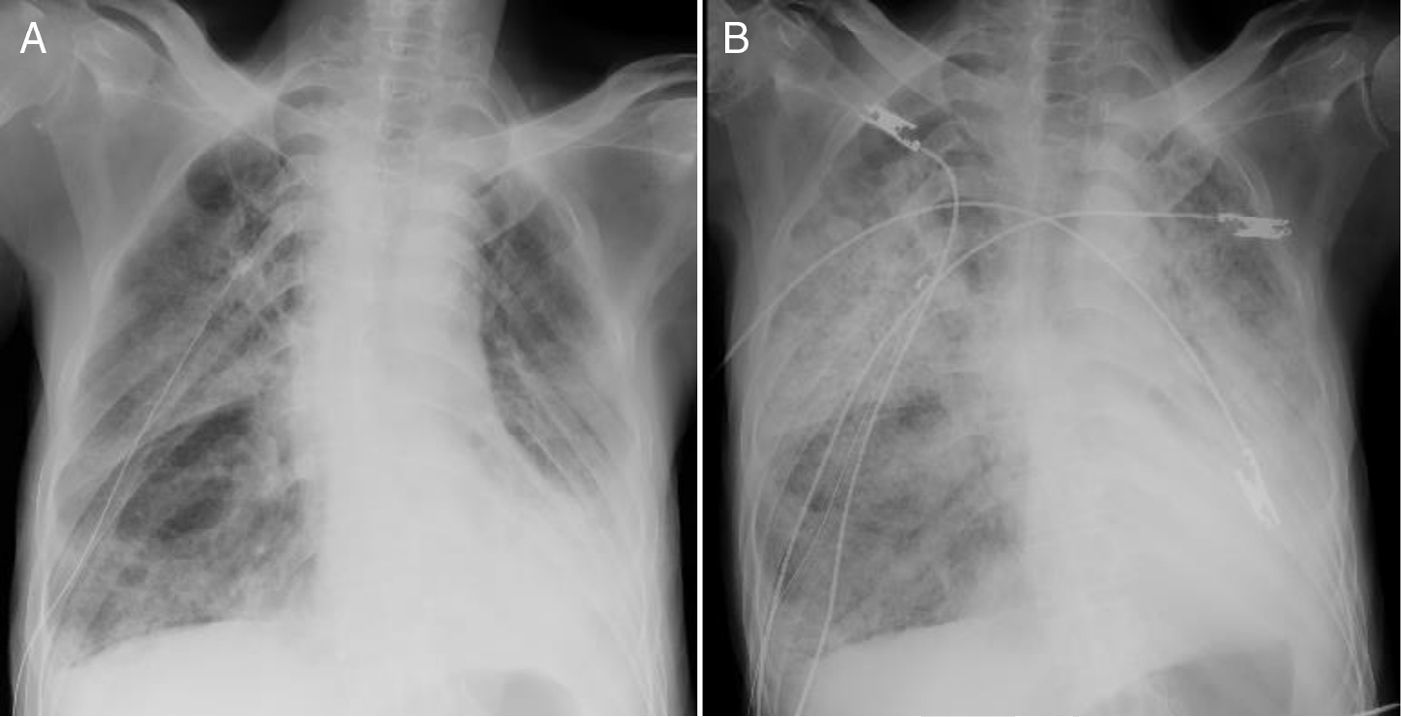
A 72-year-old man (case 1), an ex-smoker, was diagnosed with left lung adenocarcinoma (Stage IV) at 69 years of age. He had been treated with docetaxel for 1 year. A right pneumothorax was detected on follow-up computed tomography (CT), which also showed multiple blebs and severe emphysema. Thoracic drainage was performed with an 18 Fr double-lumen chest drainage tube with the application of low-pressure suction of −5cmH2O. Because of prolonged air leaks, pleurodesis was performed; 5 KE of OK-432 was primarily used. Thereafter, pleurodesis with a combination of 50ml of autologous blood and 200mg of minocycline was performed 4times. However, air leakage continued. We used 200ml of 50% glucose solution as a sclerosant, but this treatment immediately induced acute respiratory failure with hypercapnia. Chest X-ray revealed patchy consolidation in both lungs (Fig. 1), and ARDS was diagnosed, according to the Berlin definition.10 Endotracheal intubation was performed; however, the patient died from progression of respiratory failure.
An 84-year-old man (case 2), an ex-smoker, was diagnosed with idiopathic pulmonary fibrosis at 82 years of age. Home oxygen therapy had been used for chronic respiratory failure with hypercapnia for 1 year. A few days prior to admission, he had complained of chest pain and dyspnea. He was diagnosed with a right pneumothorax. Chest CT revealed honeycomb lung and multiple blebs. Thoracic drainage was performed with an 18 Fr double-lumen chest drainage tube with the application of low-pressure suction of −10cmH2O. However, air leakage continued. As pretreatment of pleurodesis, local anesthesia into the parietal pleura was performed with the injection of 20ml of 1% lidocaine into the pleural space. Thereafter, pleurodesis with 400ml of 50% glucose solution was performed, which immediately induced chest pain and the exacerbation of chronic respiratory failure with hypercapnia. Endotracheal intubation was not performed, because his family refused this treatment. After air leakage stopped, the patient died 1 week later from progression of respiratory failure.
To the best of our knowledge, this is the first report on treatment-related deaths by pleurodesis using a 50% glucose solution, which included ARDS and anaphylactic-like reaction.
Previously, 4 reports have described the effectiveness and safety of pleurodesis using a 50% glucose solution. The mechanism of this treatment is considered to be osmotic injury and inflammation caused by hypertonic glucose solution.4–7 Regarding the side effects of this treatment, previous reports have described a transient elevation in blood sugar level and rapid induction of pleural effusion.4–7 However, we witnessed 2 serious adverse effects of ARDS and anaphylactic-like reaction. Dextrose, which is another hypertonic solution, is also used as an agent of pleurodesis.8,11 Chee et al. reported on the life threatening complication of pulmonary edema caused by reflux of dextrose through a fistula into the lung tissue, as evidenced by the glucose-rich aspirate obtained from the endotracheal tube post-resuscitation.12 Although there was no evidence for this in case 1, we consider that reflux of hypertonic glucose through fistula influx into the lung tissue could have induced the serious adverse effect of ARDS. In case 2, the reason for the anaphylactic-like reaction was unknown; however, we considered that pain could have influenced such a reaction. Fujino et al. reported on the occurrence of chest pain after administration of 50% glucose solution.7 Therefore, analgesia for chest pain should be part of the pretreatment for pleurodesis using 50% glucose solution.
Clinically, a variety of sclerosants other than a 50% glucose solution have been used, including tetracyclin and its derivatives, talc, bleomycin, and OK-432, which are generally considered to be safe and convenient.2,3 However, these agents can cause serious complications of empyema, ARDS, and anaphylactic reaction, similar to this report.13–15 The choice of pleurodesis agent is heavily doctor-dependent; therefore, future studies are needed to determine which pleurodesis agents should be selected according to each patient's conditions and comorbidities.
In conclusion, there is a possibility of serious adverse reactions, including ARDS and anaphylactic-like reaction, with pleurodesis using 50% glucose solution. Therefore, pleurodesis should be performed with caution when using hypertonic 50% glucose solution.
Please cite this article as: Hamada S, Okamoto N, Watanabe I, Tsukino, M. ¿Es segura la pleurodesis con solución de glucosa al 50% en pacientes con neumotórax espontáneo? A propósito de una serie de casos. Arch Bronconeumol. 2017;53:210–211.